Dental Implant Eligibility Test Guide
Dental Implant Eligibility Test Guide to understanding your suitability for a permanent tooth replacement solution. Dental implants are widely regarded as the gold standard for replacing missing teeth, offering a level of function, stability, and aesthetics that other options cannot match. However, not everyone is an immediate candidate for this transformative procedure. The long-term success of a dental implant hinges on a series of biological and health-related factors that must be carefully evaluated by a dental professional. This evaluation, often referred to as a dental implant eligibility test, is not a single, simple exam but a comprehensive assessment of your oral and overall health to ensure the implant can integrate successfully with your body and provide a lasting result.
This in-depth process is designed to identify any potential risks or contraindications that could lead to implant failure. By thoroughly assessing factors like jawbone density, gum health, and systemic medical conditions, your dental team can create a predictable and safe treatment plan. For many patients, this may involve preparatory procedures to create an ideal environment for the implant, ensuring you have the highest possible chance of a successful outcome. Understanding these criteria is the first step toward reclaiming your smile and confidence.
What is a Dental Implant Eligibility Test?
A dental implant eligibility test is a multi-faceted diagnostic process undertaken by a dentist or oral surgeon to determine if a patient is a suitable candidate for dental implant surgery. This is not a pass-or-fail test but rather a detailed analysis of the anatomical and physiological conditions necessary for a process called osseointegration—the direct structural and functional connection between living bone and the surface of a load-bearing artificial implant. For osseointegration to occur successfully, the body must be able to heal properly and the jaw must have an adequate foundation to support the implant.
The evaluation involves several key components:
- Clinical Examination: A hands-on assessment of your teeth, gums, and overall oral cavity to check for signs of decay, gum disease, or other pathologies.
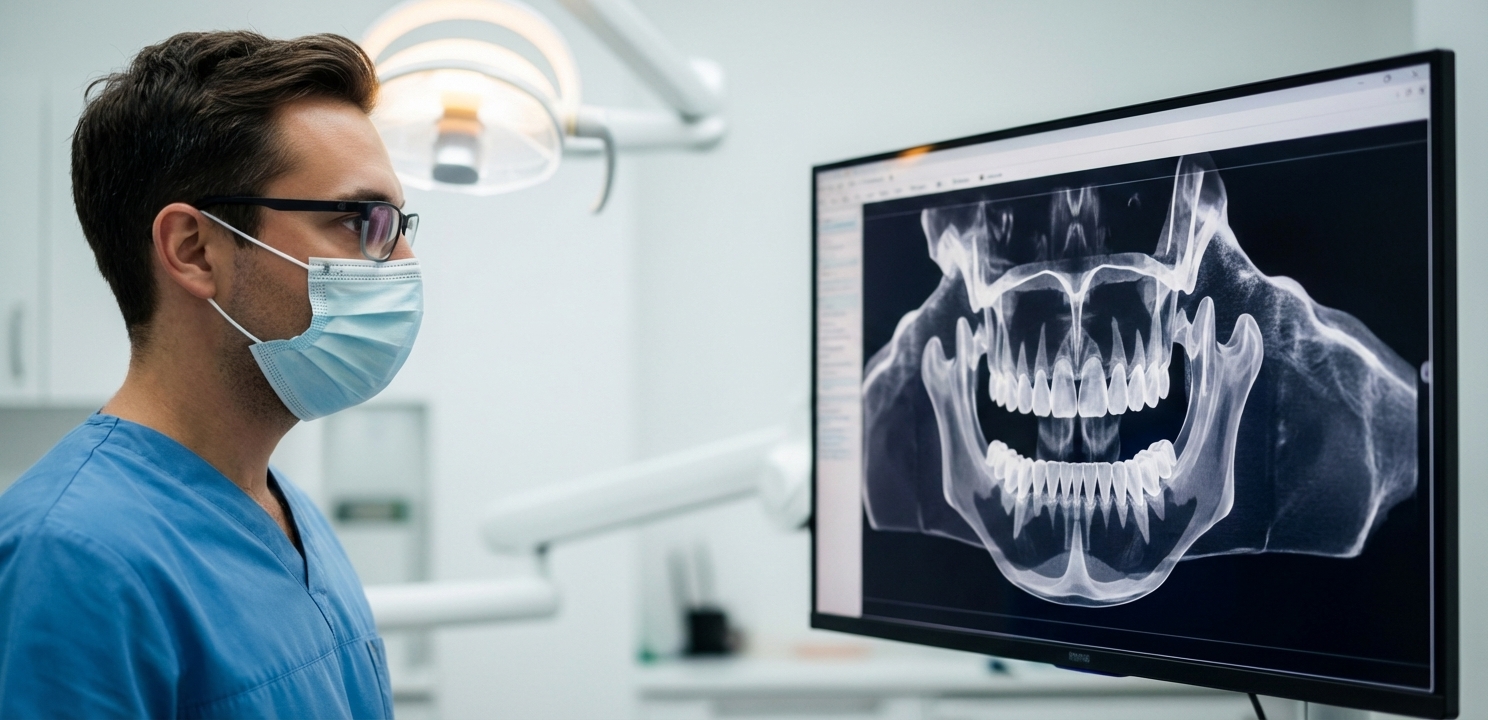
- Radiographic Imaging: This includes standard dental X-rays and, most importantly, a Cone Beam Computed Tomography (CBCT) scan. A CBCT scan provides a detailed 3D image of your jaw, allowing the dentist to measure the precise height, width, and density of the bone, as well as locate critical structures like nerves and sinuses.
- Medical History Review: A thorough discussion of your overall health, including any chronic illnesses, medications you are taking, and lifestyle habits like smoking. Certain conditions can significantly impact the body’s ability to heal and may affect the long-term prognosis of the implant.
This comprehensive approach ensures that the treatment plan is tailored specifically to your unique circumstances, maximizing the potential for a successful and durable restoration.
Key Factors Assessed During Evaluation
The success of a dental implant is dependent on a variety of interconnected factors. Your dental team will meticulously review each one to build a complete picture of your candidacy. Here are the most critical elements under consideration.
| Eligibility Factor | Ideal Condition for Implants | Potential Concern or Contraindication |
|---|---|---|
| Jawbone Density & Volume | Sufficient height and width of healthy bone to fully encase and support the implant post. | Significant bone loss (atrophy) due to prolonged tooth absence, trauma, or periodontal disease. |
| Gum (Periodontal) Health | Healthy, firm gums with no signs of inflammation, infection, or deep periodontal pockets. | Active, untreated gum disease (gingivitis or periodontitis), which can lead to peri-implantitis. |
| Overall Medical Health | Well-managed systemic health. Patient is generally healthy or has chronic conditions under control. | Uncontrolled diabetes, autoimmune disorders, osteoporosis medication (bisphosphonates), or recent radiation therapy to the head/neck. |
| Lifestyle Habits | Non-smoker, moderate or no alcohol consumption, commitment to good oral hygiene. | Heavy smoking, which constricts blood vessels and severely impairs healing. Excessive alcohol use can also hinder recovery. |
| Oral Hygiene Commitment | Patient demonstrates a strong commitment to daily brushing, flossing, and regular dental check-ups. | History of poor oral hygiene, indicating a higher risk of future implant complications like peri-implantitis. |
The Critical Role of Jawbone and Gums
Jawbone Density: The Foundation of Success
The single most important factor for dental implant eligibility is the quantity and quality of the jawbone. When a tooth is lost, the bone that once supported it begins to resorb, or shrink, due to a lack of stimulation. If a significant amount of time has passed since the tooth was lost, there may not be enough bone to securely anchor a titanium implant post. A CBCT scan is the definitive tool for assessing this, providing a three-dimensional view that reveals the exact bone dimensions. Without an adequate foundation, the implant cannot achieve the stability needed for long-term function. If your bone volume is found to be insufficient, it does not automatically disqualify you. Procedures like bone grafting for dental implants can be performed to rebuild the lost bone, creating a solid base for future implant placement.
Gum Health: Protecting the Investment
Healthy gums are essential for the longevity of a dental implant. Active periodontal disease, an infection of the gums and bone that support the teeth, must be fully treated and managed before implant surgery can proceed. The same bacteria that cause gum disease can attack the tissues around an implant, leading to a condition called peri-implantitis. Peri-implantitis can cause inflammation, bone loss around the implant, and eventual implant failure. Your dentist will conduct a thorough periodontal screening to check for deep pockets, bleeding, and other signs of infection. Establishing a healthy oral environment is a non-negotiable prerequisite for this advanced treatment.
Systemic Health and Lifestyle Considerations
Your overall health plays a direct role in your body’s ability to heal from surgery and integrate the dental implant. Certain medical conditions and medications can interfere with this process. For instance, patients with uncontrolled diabetes experience slower healing and have a higher risk of infection, which can compromise osseointegration. A comprehensive review by the National Center for Biotechnology Information highlights that while well-controlled diabetes is not an absolute contraindication, poor glycemic control is a significant risk factor. Similarly, autoimmune diseases that affect wound healing or medications that suppress the immune system must be carefully considered.
Lifestyle habits, particularly smoking, are a major concern. The nicotine and other chemicals in tobacco smoke restrict blood flow to the gums and bone, depriving the surgical site of the oxygen and nutrients needed for healing. This significantly increases the risk of implant failure. Heavy alcohol consumption can also negatively impact healing. Being transparent with your dental surgeon about your medical history and lifestyle is crucial for a safe and successful procedure.
The Pathway to Eligibility: What if You’re Not a Candidate Yet?
Receiving news that you are not an immediate candidate for dental implants can be disheartening, but it is rarely the end of the road. Modern dentistry offers several advanced procedures designed to address the very issues that might initially prevent implant placement. These preparatory treatments are designed to build the ideal foundation for success.
Addressing Bone Deficiencies
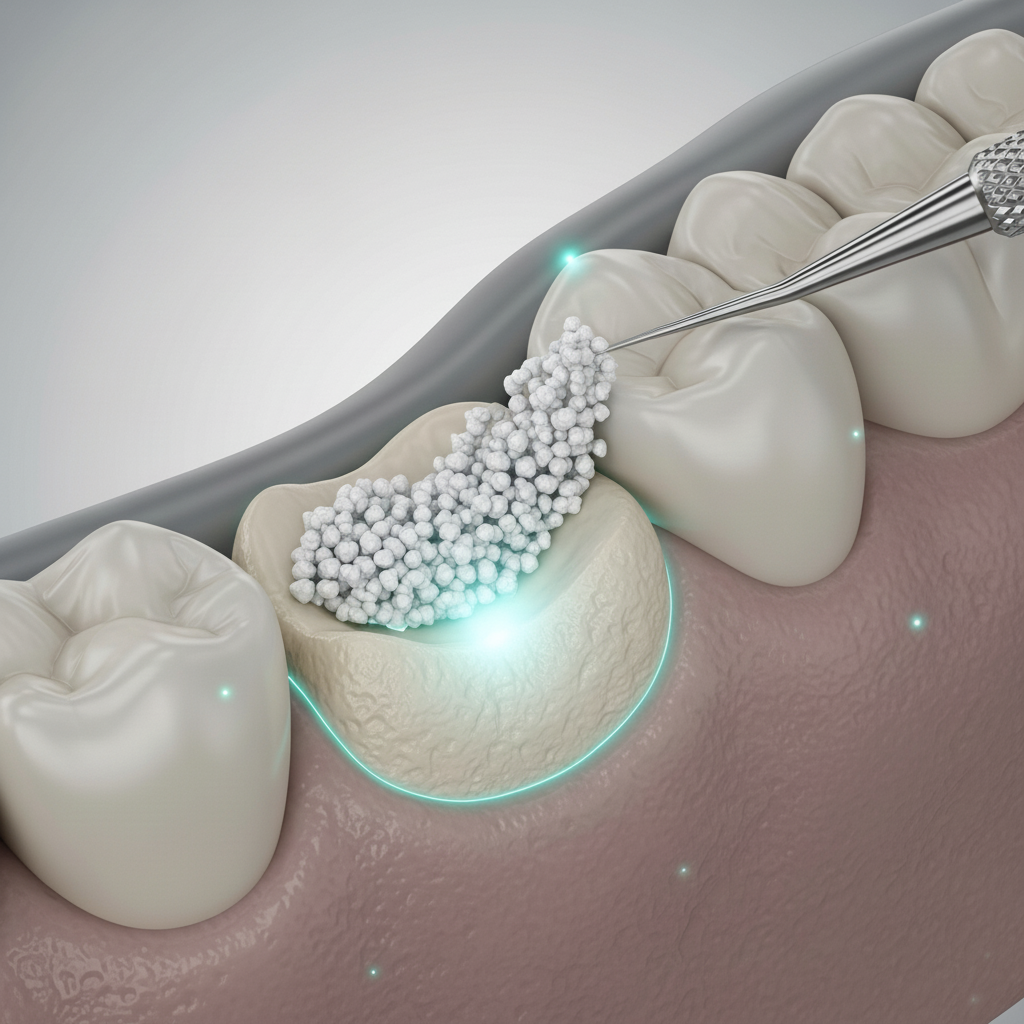
For patients with insufficient jawbone, bone grafting is a common and highly effective solution. This procedure involves adding bone material (either from your own body, a donor source, or a synthetic material) to the deficient area. Over several months, this material integrates with your natural bone, creating a stronger and more voluminous site capable of supporting an implant. For the upper jaw, where the sinus cavity can limit available bone height, a sinus lift procedure may be recommended. This involves gently raising the sinus membrane and placing a bone graft underneath it to create the necessary vertical height for implant placement.
Managing Oral and Systemic Health
If active gum disease is present, a course of periodontal therapy will be the first step. This may include deep cleanings (scaling and root planing) to remove plaque and tartar below the gumline and, in some cases, antibiotic treatment. Only once the infection is resolved and gum health is stable can implant surgery be considered. For systemic health issues, your dental surgeon will often work in collaboration with your primary care physician to ensure any conditions, like diabetes, are well-managed and stable before proceeding with surgery. By taking these preliminary steps, many patients who were initially deemed unsuitable can become excellent candidates for dental implants.





