Dental Implant Healing Month by Month

Dental Implant Healing Month by Month is a journey of transformation, a biological process where a titanium post becomes a part of your own jawbone, creating a permanent foundation for a new tooth. Understanding this timeline is not just about satisfying curiosity; it’s a crucial part of being an active and informed participant in your own oral health success. The path to a fully restored, functional, and beautiful smile follows a predictable, albeit patient, schedule dictated by your body’s incredible ability to heal and integrate a foreign material. From the initial hours after surgery to the moment your final crown is placed, each phase has unique milestones, care requirements, and sensations. This guide provides a comprehensive overview of what to expect, empowering you with the knowledge to navigate your recovery with confidence and ensure the long-term success of your investment.
The Critical First Month: Laying the Foundation for Success
The first 30 days post-surgery are the most intensive period of healing. This is when the soft tissues mend and the initial groundwork for bone fusion is established. Diligent aftercare during this month is paramount to prevent complications and set the stage for a smooth recovery process.
The First 24-48 Hours: Managing the Immediate Aftermath
Immediately following your implant placement surgery, your primary focus will be on managing discomfort, swelling, and minor bleeding. It’s normal to experience some oozing from the surgical site; this can be controlled by gently biting on a clean gauze pad. Swelling typically peaks around the 48-to-72-hour mark. Applying a cold pack to the outside of your face in 20-minute intervals can significantly reduce inflammation and provide relief. Your surgeon will prescribe pain medication, which you should take as directed to stay ahead of any discomfort. Your diet must consist exclusively of soft, cool foods like yogurt, smoothies, and lukewarm soups. Avoid hot liquids, alcohol, and smoking, as these can interfere with blood clotting and irritate the sensitive tissues. Rest is essential; avoid any strenuous activity that could elevate your blood pressure and increase bleeding.
Week 1-2: Soft Tissue Healing and Initial Adaptation
As you move into the first and second weeks, you’ll notice a gradual reduction in swelling and discomfort. The surgical site will begin to look and feel much better as the gum tissue heals. If you have non-dissolvable sutures, they are typically removed around 7-14 days after the procedure. Oral hygiene is critical but must be performed with extreme care. You can begin to gently rinse your mouth with a prescribed antimicrobial mouthwash or a warm salt-water solution several times a day, especially after meals. You should brush your other teeth normally but avoid the surgical area entirely to prevent disturbing the implant. Your diet can expand slightly to include softer solid foods like scrambled eggs, mashed potatoes, and well-cooked pasta, but you must continue to avoid chewing near the implant site.
Week 3-4: The Quiet Beginning of Osseointegration
By the end of the first month, the visible signs of surgery should have largely subsided. Your gums will appear healed, and you should be experiencing little to no pain. While it may seem like the healing is complete, the most important work is just beginning beneath the surface. This is when the initial stages of osseointegration commence, where your jawbone starts to grow onto and fuse with the titanium implant. You will likely feel quite normal, but it is imperative to remember that the implant is not yet stable. You must continue to avoid placing any direct chewing pressure on the implant. Any premature force can disrupt the delicate process of bone integration and risk implant failure. Continue with meticulous but gentle oral hygiene and slowly reintroduce more foods into your diet, always being mindful of the healing site.
Dental Implant Healing Month by Month Timeline Explained
The journey from a newly placed implant to a fully functional tooth is a multi-stage process. While individual healing rates can vary based on factors like overall health, bone quality, and the complexity of the procedure, a general timeline provides a reliable roadmap. This table breaks down the key phases, offering a clear overview of what to expect as your body works to create a permanent bond with your new implant.
| Timeframe | Key Milestones & Sensations | Dietary Guidelines | Oral Hygiene & Activity |
|---|---|---|---|
| Month 1 | Initial soft tissue healing. Swelling and discomfort subside. Sutures may be removed. Osseointegration begins. Minimal sensation at the implant site itself. | Liquid to very soft diet for the first two weeks (soups, smoothies, yogurt). Gradually introduce softer solids (eggs, pasta, fish). Avoid chewing on the implant. | Gentle warm salt-water rinses. Avoid the surgical site when brushing. No strenuous physical activity for the first 1-2 weeks. |
| Month 2 | Bone cells actively growing and attaching to the implant surface. No significant external changes. The implant remains undisturbed under the gum. | Continue to favor the other side of the mouth for chewing. Firmer foods can be eaten, but avoid very hard, crunchy, or sticky items. | Normal brushing and flossing can resume for all other teeth. Continue to be gentle around the implant area. Light to moderate exercise is usually fine. |
| Month 3 | Osseointegration is well underway. The implant is becoming more stable within the jawbone. The risk of early failure significantly decreases. | Diet continues to normalize. While still avoiding direct, forceful chewing on the implant, you can eat a wider variety of textures. | Maintain excellent oral hygiene. Regular check-ups may be scheduled to monitor progress. |
| Months 4-6+ | Osseointegration is complete or nearing completion. The implant is now rigidly fixed in the bone. A follow-up appointment will confirm stability. | Most dietary restrictions are lifted after the dentist confirms successful integration. You can begin to use the area more normally. | Preparation for the final restoration (abutment and crown) begins. Once the crown is placed, treat it like a natural tooth with regular brushing and flossing. |
Months 2-3: The Silent Work of Osseointegration
This phase is often called the “quiet” period of healing. On the surface, not much appears to be happening. You will likely feel completely normal, with no pain or discomfort. However, this is arguably the most critical stage of the entire process. Beneath your healed gums, a microscopic marvel of biology is taking place as your jawbone permanently fuses with the implant.
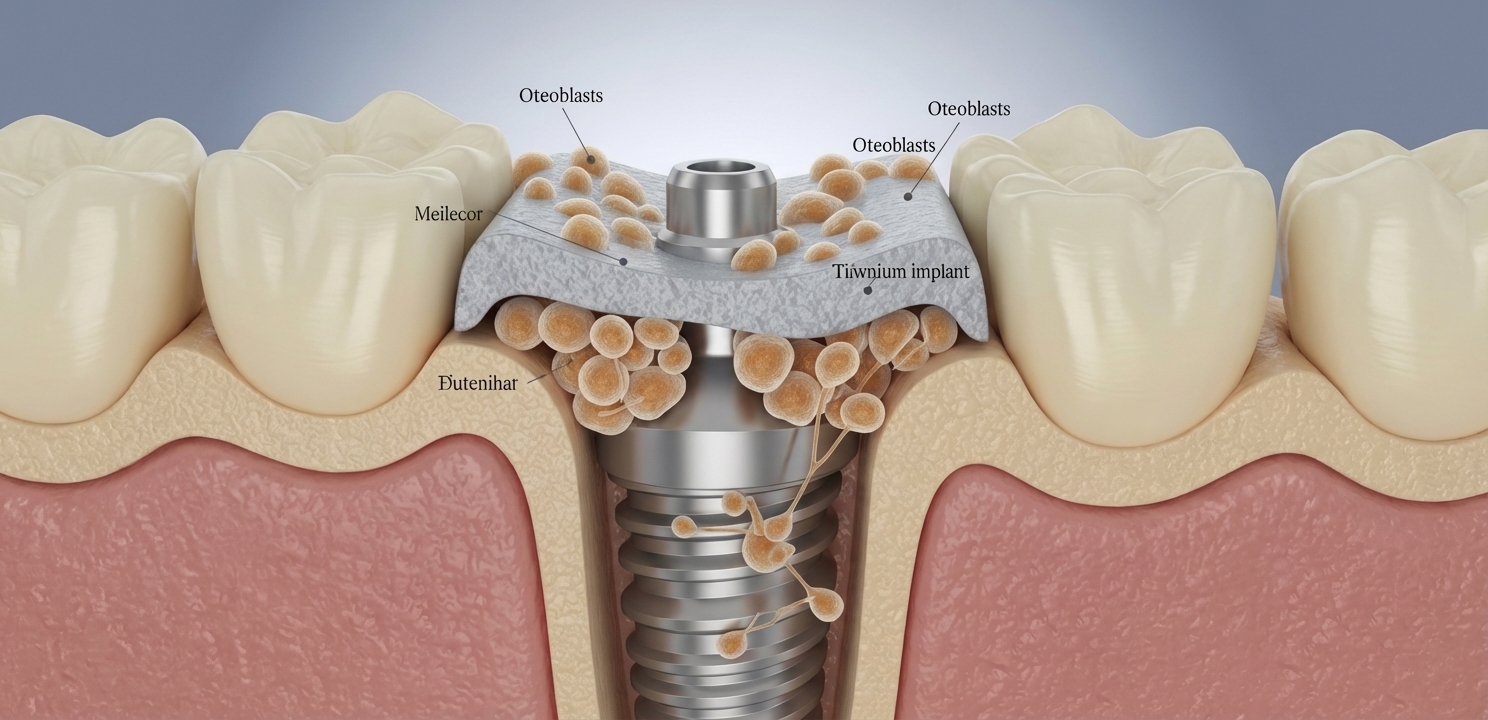
What is Osseointegration?
Osseointegration is the biological process that allows dental implants to be a successful long-term solution for tooth replacement. It refers to the direct structural and functional connection between living bone and the surface of a load-bearing artificial implant. The titanium used for dental implants is exceptionally biocompatible, meaning the body does not recognize it as a foreign invader and does not mount an immune response against it. Instead, specialized bone cells called osteoblasts migrate to the implant’s surface, which is often micro-textured to increase surface area. These cells deposit new bone matrix directly onto the titanium, gradually locking it into place. This powerful bond is what gives a dental implant its incredible strength and stability, allowing it to withstand the same chewing forces as a natural tooth root. The entire process is a testament to the body’s remarkable regenerative capabilities, as detailed in extensive scientific literature on the subject. A thorough review in the Journal of Indian Prosthodontic Society explains this complex cellular interaction in great detail.
Months 4-6: Achieving Stability and Preparing for Restoration
As you enter the final months of the initial healing period, the process of osseointegration is nearing completion. The implant, once a separate component, is now functionally a part of your jaw. This newfound stability is the green light for moving on to the final, restorative phase of your treatment—getting your new tooth.
Verifying Implant Success
Before proceeding, your dentist must confirm that the implant has fully and successfully integrated with the bone. This is a crucial checkpoint to ensure the foundation is solid enough to support a crown and withstand daily chewing forces. This verification is typically done in two ways. First, a dental X-ray will be taken to visually inspect the bone level around the implant threads. Healthy, dense bone surrounding the implant is a clear sign of success. Second, the surgeon may perform a gentle stability test. This can involve attempting to wiggle the implant (it should have zero mobility) or using a specialized torque wrench to apply a specific, measured amount of rotational force. If the implant remains immovable, it has passed the test, and you are ready for the next step. If you’re looking for an even more detailed breakdown of the initial healing period, you can find more information in our dental implant recovery day by day guide.
The Abutment and Crown Phase
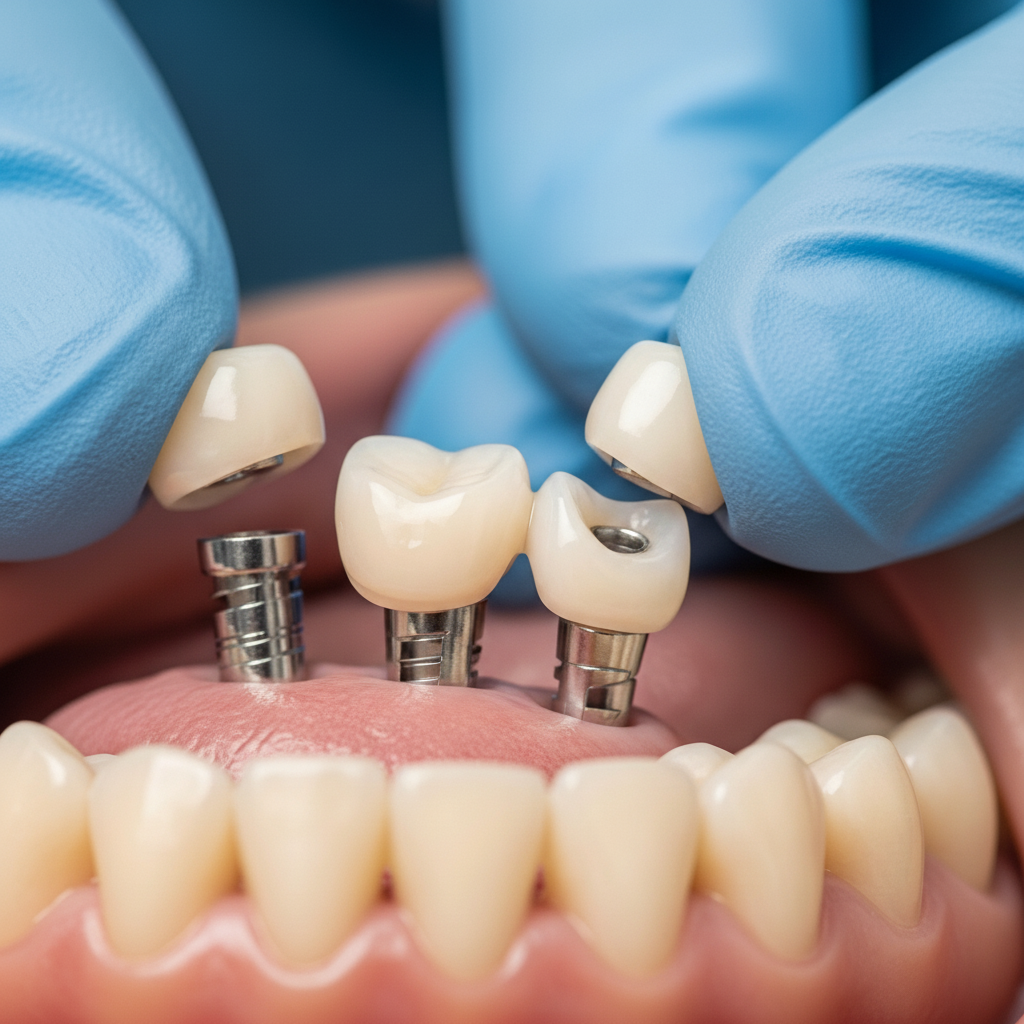
Once successful integration is confirmed, the restorative phase begins. This often requires a second, much smaller procedure to expose the top of the implant and attach a connector piece called an abutment. The abutment serves as the link between the implant in your jaw and the final crown that will be visible in your mouth. After the abutment is in place and the gums have healed around it for a week or two, your dentist will take precise impressions of your mouth. These impressions are sent to a dental laboratory where your custom crown is meticulously fabricated to match the color, shape, and size of your surrounding natural teeth. At your final appointment, this crown is permanently attached to the abutment, completing the process and fully restoring your smile and function.






