Best Dental Implant Method for Success
Best Dental Implant Method for Success is one that combines advanced technology, superior materials, and a personalized treatment plan tailored to your unique anatomical and aesthetic needs. The journey to restoring a complete, functional, and beautiful smile is a significant one, and choosing the right approach is the cornerstone of a lasting outcome. While the concept of a single “best” method is subjective and depends heavily on individual circumstances, modern dentistry offers a range of highly effective solutions, each designed to address specific patterns of tooth loss, from a single missing tooth to a full arch replacement. Understanding these methods, their underlying principles, and the factors that contribute to their high success rates empowers you to make an informed decision alongside your dental surgeon.
At the core of every successful dental implant is a remarkable biological process. This process ensures the implant becomes a permanent, stable part of your jaw, capable of withstanding the immense forces of biting and chewing for decades. This foundation is non-negotiable for long-term implant viability and is the primary reason why implants are considered the gold standard for tooth replacement.
Understanding the Foundation of Dental Implants: Osseointegration
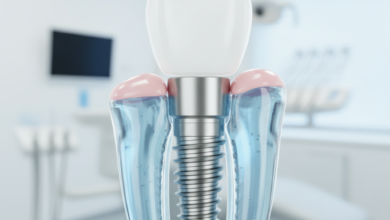
Before comparing different implant methods, it is crucial to understand the scientific principle that makes them all possible: osseointegration. This term describes the direct structural and functional connection between living bone and the surface of a load-bearing artificial implant. Dental implants are typically made from commercially pure, medical-grade titanium or a titanium alloy. This material is biocompatible, meaning the human body does not recognize it as a foreign object and will not reject it. When a titanium implant is surgically placed into the jawbone, a healing process begins. Over a period of several months, bone cells migrate to the implant’s surface, growing into its microscopic irregularities and fusing directly with the metal. This fusion creates an incredibly strong and stable anchor, essentially making the implant a synthetic tooth root. The success of this process is paramount; without complete osseointegration, the implant will fail. Factors that influence successful osseointegration include the patient’s overall health, bone quality and quantity, surgical technique, and the absence of infection. A skilled surgeon ensures the implant is placed with precision to maximize initial stability, creating the optimal environment for the bone to heal and integrate around it.
Comparing Modern Dental Implant Solutions
The application of dental implants ranges from replacing a single lost tooth to reconstructing an entire dental arch. The best method for a patient is determined after a thorough evaluation that includes 3D CBCT scans, an assessment of bone density, and a discussion of the patient’s functional and aesthetic goals. The primary categories of implant solutions are single-tooth implants and full-arch restorations, often known by the term “All-on-X.”
Single Tooth Implants: The Gold Standard for Individual Gaps
When a single tooth is lost due to trauma, decay, or disease, a single dental implant is often the ideal solution. This method involves placing one implant into the jawbone at the site of the missing tooth. After the osseointegration period, an abutment (a connector piece) is attached to the implant, and a custom-fabricated crown is secured to the abutment. The primary advantage of this approach is its conservative nature. Unlike a traditional dental bridge, a single implant does not require the grinding down of healthy adjacent teeth for support. This preserves natural tooth structure and promotes better long-term oral health. Furthermore, the implant stimulates the surrounding jawbone, preventing the bone loss that naturally occurs when a tooth root is no longer present. The result is a replacement tooth that looks, feels, and functions just like a natural one, providing a seamless and durable restoration.
Full-Arch Solutions: The All-on-X Revolution
For patients who are missing most or all of their teeth in an upper or lower arch (edentulism), full-arch restoration systems like All-on-4, All-on-6, or All-on-8 offer a transformative solution. These methods provide a fixed, non-removable bridge supported by a strategically placed number of implants. The “All-on-4” concept, for example, utilizes four implants, with the posterior implants typically placed at an angle. This angulation is a key innovation, as it allows the implants to engage more of the patient’s existing bone, often avoiding the need for extensive bone grafting procedures. All-on-6 and All-on-8 add more implants for increased support and load distribution, which may be recommended for patients with lower bone density or those who desire maximum stability. These full-arch solutions provide immediate improvements in chewing ability, speech, and aesthetics, often allowing a patient to leave the day of surgery with a temporary but functional set of teeth.
What is the Best Dental Implant Method? A Detailed Comparison
Choosing between implant strategies requires weighing several factors. The following table provides a clear comparison between the primary methods to help illustrate which might be most suitable for different clinical situations. This is a critical step in a patient’s journey, and a comprehensive full mouth implants total cost guide can provide further clarity on the investment involved in these life-changing procedures.
| Feature | Single Implants | All-on-4 / All-on-6 |
|---|---|---|
| Ideal Candidate | Patient missing one or several non-adjacent teeth with sufficient bone at each site. | Patient missing most or all teeth in an arch (edentulous or near-edentulous). |
| Number of Implants | One implant per missing tooth. | 4, 6, or 8 implants to support an entire arch of 10-14 teeth. |
| Bone Grafting Likelihood | Moderate to high if bone loss has occurred at the specific tooth site. | Lower, as angled posterior implants are designed to utilize available bone more efficiently. |
| Procedure Duration | Shorter surgical time per implant, but multiple surgeries if many teeth are replaced. | A single, more complex surgery to place all implants for one arch. |
| Healing & Integration | 3-6 months of osseointegration before the final crown is placed. | 3-6 months of osseointegration, but often a temporary fixed bridge can be worn immediately. |
| Final Prosthesis | Individual dental crown for each implant. | A full-arch bridge (made of acrylic, zirconia, or other materials) fixed to the implants. |
| Overall Treatment Time | Can be lengthy if multiple implants are placed and healed in stages. | Generally faster for a full-smile restoration, from surgery to final prosthesis. |
The Critical Role of Technology and Materials
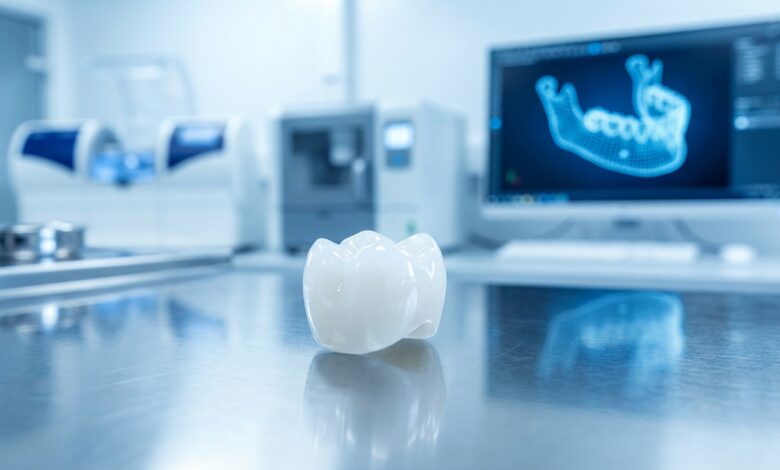
The success of any dental implant procedure is heavily dependent on the quality of the materials used and the precision of the diagnostic and surgical process. Top-tier clinics utilize implants from globally recognized manufacturers known for their extensive research and high success rates. The material for the final restoration is equally important. While traditional porcelain-fused-to-metal (PFM) crowns are an option, modern materials like Zirconia and E-max offer superior strength, durability, and aesthetics. Zirconia is exceptionally strong and resistant to chipping, making it ideal for full-arch bridges, while E-max provides outstanding translucency for a highly natural look, perfect for front teeth.
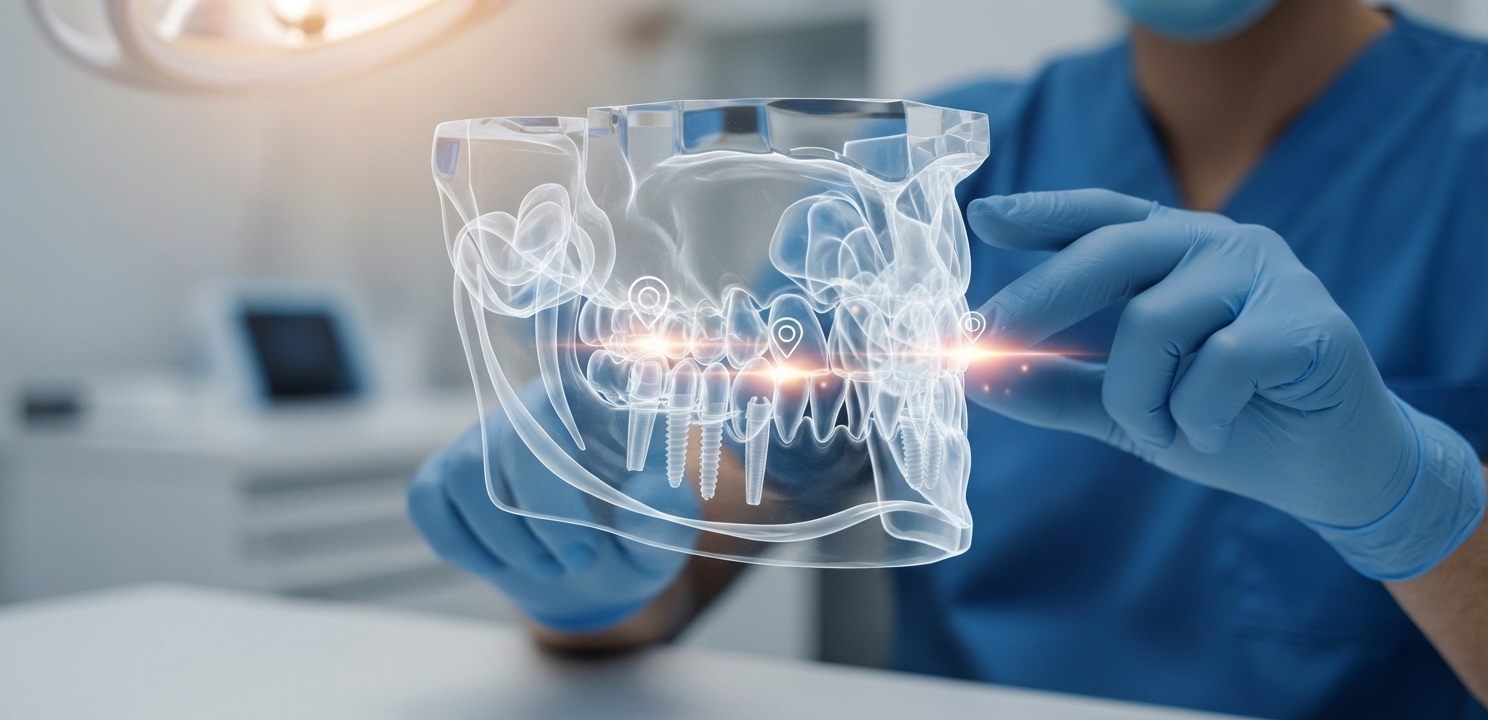
Advanced diagnostic technology, particularly Cone Beam Computed Tomography (CBCT), is non-negotiable for modern implant planning. A 3D CBCT scan provides a detailed, multi-angled view of the jawbone, nerves, and sinus cavities. This allows the surgeon to virtually plan the exact position, angle, and depth of each implant before the surgery even begins. This digital planning minimizes risks, ensures optimal placement for bone support, and leads to more predictable and safer outcomes.
The Treatment Process: A Step-by-Step Guide
The path to a new smile with dental implants follows a structured, multi-stage process designed to ensure the highest chance of success and longevity.
Initial Consultation and Planning
This first step is the most critical. It involves a comprehensive dental examination, a review of your medical history, and the crucial 3D CBCT scan. During this phase, your surgeon will assess your bone structure, discuss your goals, and determine the most appropriate implant method for you. A detailed, personalized treatment plan is then created, outlining every step of the process.
The Surgical Procedure
Implant placement is a surgical procedure performed under local anesthesia, with sedation options available for patient comfort. The surgeon makes a small incision in the gum tissue to access the bone, then uses a series of precise drills to create the space for the implant. The implant is then carefully screwed into place, and the gum tissue is sutured. For All-on-X cases, all necessary implants for the arch are placed during this single appointment.
Healing and Osseointegration
Following surgery, the crucial osseointegration period begins. This typically lasts from three to six months. During this time, the jawbone fuses with the implants. It is vital to follow all post-operative instructions, maintain excellent oral hygiene, and avoid placing excessive force on the implants to ensure this process is not disrupted.
Final Restoration
Once osseointegration is complete and confirmed, the final phase begins. This involves taking precise impressions or digital scans of your mouth and the position of the implants. These models are sent to a dental laboratory where your final custom crown or bridge is meticulously fabricated. Once ready, the final prosthesis is securely attached to the implants, completing your new, permanent smile. The result is a restoration that is not only beautiful but also fully functional, allowing you to eat, speak, and smile with renewed confidence.