How to Fix a Failed Dental Implant
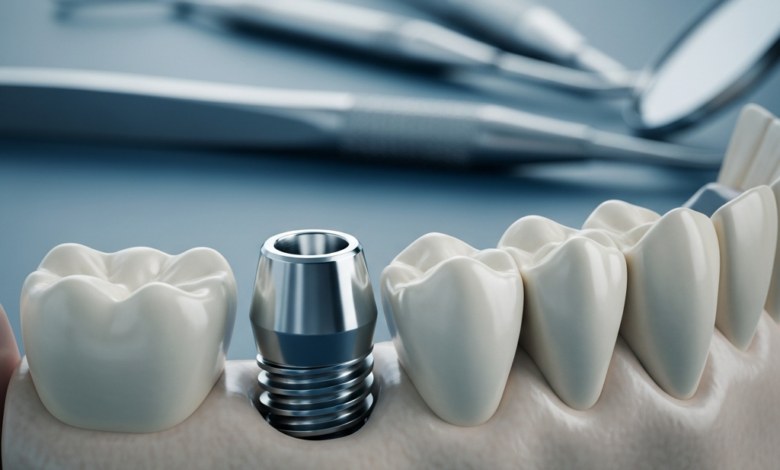
Dental implants are widely regarded as the gold standard for replacing missing teeth, boasting an impressive success rate of over 95%. They offer a permanent, stable, and aesthetically pleasing solution that can last a lifetime. However, in a small percentage of cases, complications can arise, leading to what is known as a failed dental implant. While this can be a distressing experience for a patient who has invested time and resources into the procedure, it is crucial to understand that it is often a correctable situation. With proper diagnosis and expert intervention, a new path forward can be established to restore both function and confidence in your smile.
How to Fix a Failed Dental Implant
Understanding Dental Implant Failure: Early vs. Late Stage
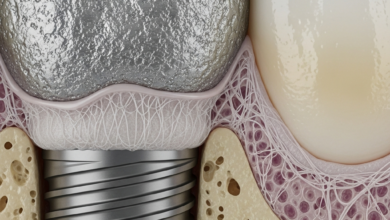
The success of a dental implant hinges on a biological process called osseointegration, where the titanium implant post fuses directly with the jawbone. This fusion creates the strong and stable foundation needed to support a dental crown. Implant failure is typically categorized based on when it occurs in relation to this critical process: early-stage failure or late-stage failure.
Early Implant Failure
Early-stage failure happens within the first three to four months following the surgical placement of the implant post. This type of failure is almost always related to a disruption or complete lack of osseointegration. The implant simply does not bond with the surrounding bone. Several factors can contribute to this outcome:
- Infection: An infection developing at the surgical site can prevent healing and hinder the bone’s ability to fuse with the implant. This can stem from pre-existing bacteria or contamination during the procedure.
- Insufficient Bone Volume or Quality: Implants require a certain density and volume of jawbone to anchor securely. If the bone is too soft or there isn’t enough of it, osseointegration may not occur successfully.
- Surgical Technique: The skill of the surgeon is paramount. Overheating the bone during the drilling process or improper positioning of the implant can damage the surrounding bone cells and lead to failure.
- Premature Loading: Placing a permanent crown and exposing the implant to chewing forces before it has fully integrated can disrupt the delicate healing process, causing micromovement that prevents fusion.
- Systemic Health Factors: Certain uncontrolled medical conditions, such as diabetes or autoimmune disorders, can impair the body’s healing capacity and increase the risk of early failure.
Late Implant Failure
Late-stage failure occurs a year or more after the implant has been successfully placed and has fully integrated with the jawbone. In these cases, the initial procedure was successful, but new problems have developed over time. The primary causes of late failure include:
- Peri-implantitis: This is the most common cause of late implant failure. It is an inflammatory condition, similar to gum disease (periodontitis), that affects the tissues and bone around an implant. It is caused by bacterial plaque buildup and, if left untreated, leads to progressive bone loss and the eventual loosening of the implant.
- Excessive Biting Forces: While implants are strong, they are not immune to extreme forces. Chronic teeth grinding (bruxism) or a misaligned bite can place immense and repeated stress on the implant and the surrounding bone, potentially causing the implant or its components to fracture or the bone to recede.
- Poor Oral Hygiene: Neglecting proper cleaning allows harmful bacteria to accumulate around the implant, leading directly to peri-implantitis. Consistent and thorough oral hygiene is non-negotiable for the long-term health of an implant.
- Mechanical Failure: Though rare with modern, high-quality implants, the implant post, abutment (connector piece), or the crown can sometimes break or loosen due to trauma or material fatigue over many years.
–
| Feature | Early-Stage Failure | Late-Stage Failure |
|---|---|---|
| Timing | Within 3-4 months post-surgery | One year or more after placement |
| Primary Cause | Failure of osseointegration | Loss of existing osseointegration |
| Common Triggers | Surgical site infection, poor bone quality, premature loading, poor healing | Peri-implantitis, poor oral hygiene, excessive bite forces, mechanical issues |
| Key Indicator | Implant never becomes stable | A previously stable implant becomes loose |
Recognizing the Signs of a Failed Dental Implant
Identifying the warning signs of implant failure is the first step toward getting the necessary treatment. While some minor discomfort and swelling are normal immediately after surgery, persistent or newly developing symptoms should be evaluated by a dental professional immediately. These signs of a failed dental implant can range from subtle to severe.
Key Symptoms to Watch For
Pain and Discomfort: While post-operative pain is expected, pain that is severe, throbbing, or worsens over time is a major red flag. Pain that appears months or years after the procedure is also abnormal.
Gum Inflammation and Swelling: Red, swollen, or tender gums around the implant site are often the first sign of an infection like peri-implantitis. The gums may also bleed easily when brushing.
Implant Mobility: A successfully integrated dental implant should feel as solid and immovable as a natural tooth. Any perceptible wiggle or looseness in the implant post itself (not just the crown) indicates a serious problem with osseointegration.
Difficulty Chewing or Biting: Pain or a strange sensation when you bite down can indicate that the implant is loose or that there is inflammation in the surrounding tissues.
Pus or Discharge: The presence of pus coming from the gumline around the implant is a definitive sign of infection that requires immediate attention.
Gum Recession: If the gums begin to pull away from the implant, exposing the metal post, it is often a sign of underlying bone loss.
The Diagnostic and Treatment Process for a Failed Implant
If you suspect your implant is failing, a thorough evaluation by an experienced dental surgeon is essential. The diagnostic process is systematic and designed to identify the exact cause and extent of the problem to formulate the most effective treatment plan.
Step 1: Clinical Examination and Imaging
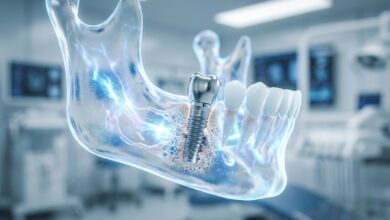
The first step involves a comprehensive physical examination. Your dentist will visually inspect the implant site for signs of inflammation, check for any mobility, and use a periodontal probe to measure the depth of the gum pockets around the implant. Deep pockets are a sign of bone loss. Following the physical exam, dental X-rays are crucial. A series of periapical X-rays or a more detailed Cone Beam Computed Tomography (CBCT) scan will be taken to get a clear picture of the bone level and structure surrounding the implant post.
Step 2: Treatment Options
The appropriate treatment depends entirely on the cause and severity of the failure. In some minor cases, the implant can be saved. For instance, if only the crown is loose, it may just need to be re-tightened or re-cemented. If early-stage gum inflammation (peri-mucositis) is present, a deep professional cleaning and a strict at-home hygiene regimen may be enough to reverse it. However, if significant bone loss has occurred or the implant is mobile, removal is often the only viable option.
The Procedure for Removing and Replacing a Failed Dental Implant
Implant Removal and Site Debridement
The surgeon will use specialized instruments to carefully detach the implant from the bone. Once removed, the entire area is thoroughly cleaned to remove all infected and inflamed tissue. This debridement is critical to creating a healthy environment for healing and eliminates the source of the problem that caused the failure.
Bone Grafting and Healing
Implant failure is almost always associated with some degree of bone loss. To create a solid foundation for a new implant, this lost bone must be rebuilt. This is accomplished through a bone grafting procedure. As detailed in numerous studies on implant dentistry, bone grafting is a predictable way to regenerate lost bone. According to a review from the National Center for Biotechnology Information, various grafting materials can be used to augment the bone, providing the necessary volume and density for future implant success. After the graft is placed, a healing period of several months is required for the new bone to mature and integrate.
Placing a New Implant
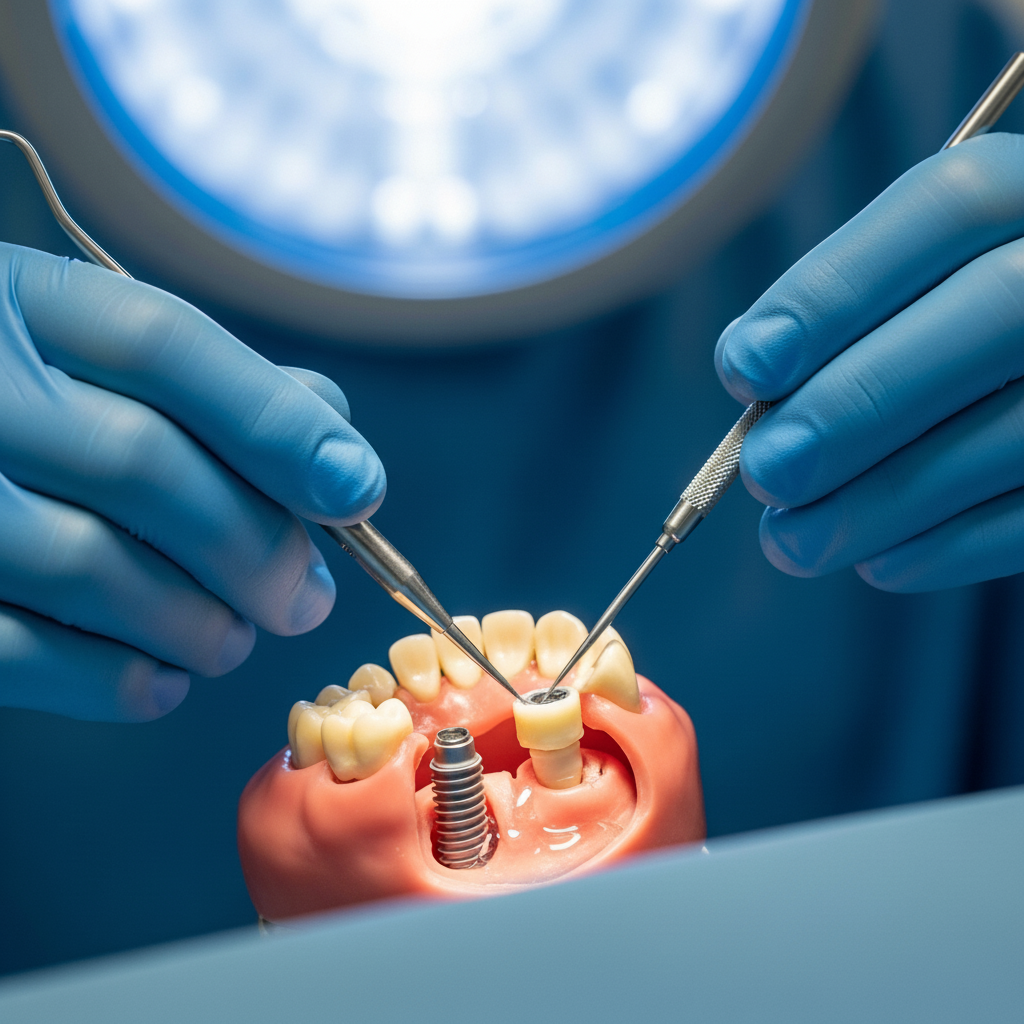
Once the jawbone has fully healed and is deemed strong enough, a new dental implant can be placed. The success rate for a replacement implant is very high, provided the original cause of failure has been addressed and the patient is committed to excellent oral hygiene. This multi-stage process, while lengthy, offers patients a second chance at a permanent and successful tooth replacement.