Dental Implant Complications Explained
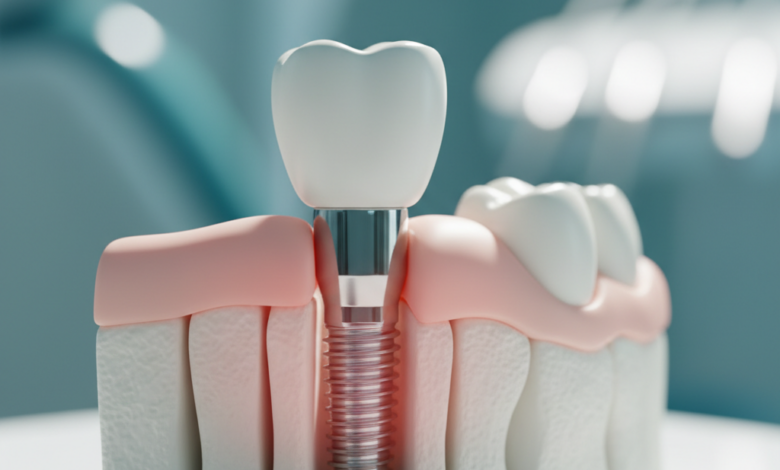
Early-stage complications typically arise within the first few months following the implant placement surgery. These are often related to the surgical procedure itself or the initial healing response of the body. One of the most common concerns is a post-operative infection at the surgical site. While minor swelling and discomfort are normal, persistent pain, discharge, or fever can indicate an an infection that requires immediate attention with antibiotics. Another potential issue is nerve damage, which can result in tingling, numbness, or pain in the surrounding gums, lips, or chin. This is a rare occurrence when proper pre-operative imaging, such as a CBCT scan, is used to map the precise location of nerves. For implants placed in the upper jaw, there is a risk of sinus perforation if the implant extends into the sinus cavity, which may require a subsequent procedure to correct. Finally, the primary stability of the implant is paramount. If the implant is not sufficiently stable in the bone at the time of placement, it may fail to integrate properly, a condition known as early implant failure.
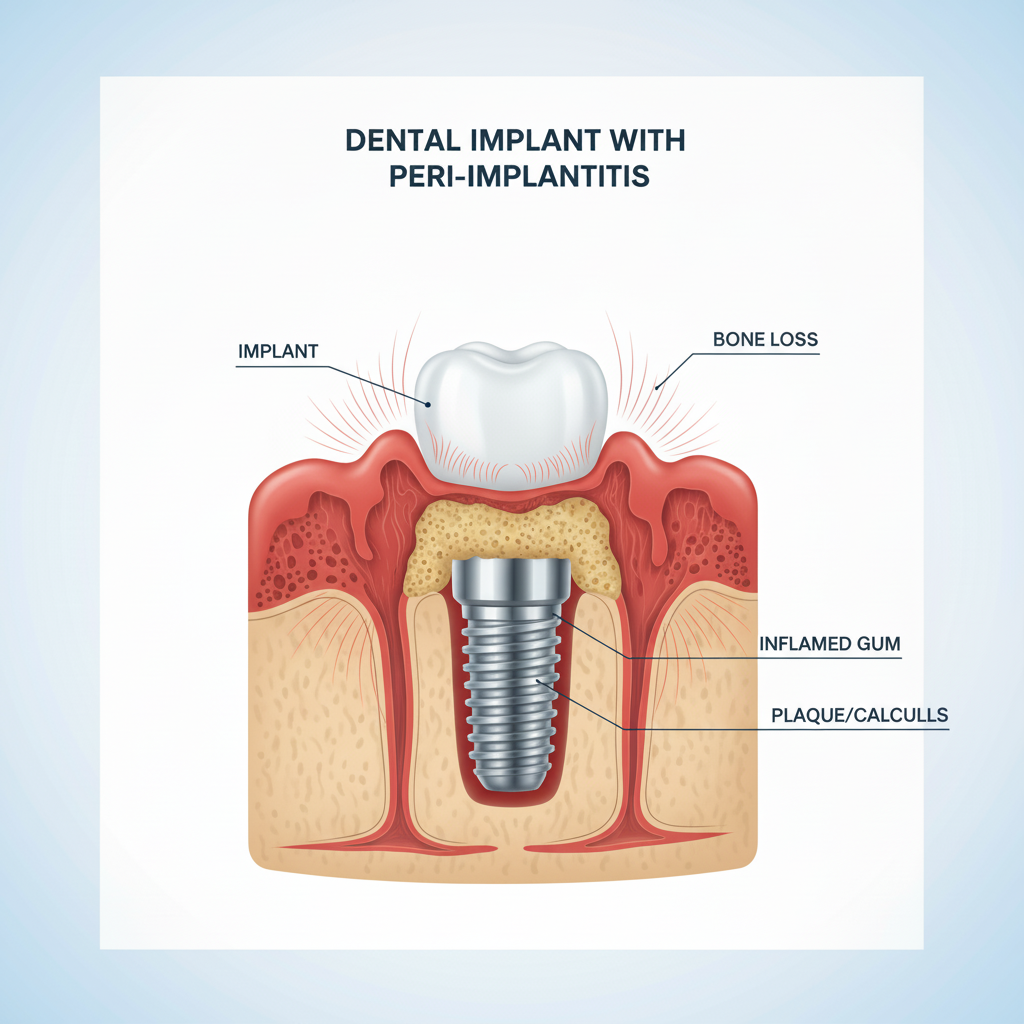
Dental Implant Complications Explained. While dental implants are celebrated for their remarkably high success rate and ability to restore function and aesthetics, it is crucial for patients to understand that, like any surgical procedure, they are not entirely without potential issues. Acknowledging and understanding these potential complications is the first and most critical step towards prevention and successful, long-term outcomes. The journey to a restored smile is a partnership between a skilled clinical team and an informed patient. By exploring the nature of these complications, their causes, and their remedies, patients can be better equipped to ensure the longevity of their investment in their oral health.
The vast majority of dental implant procedures are successful, with long-term success rates often cited as being over 95%. This statistic is a testament to the advancements in dental technology, materials, and surgical techniques. However, the small percentage of cases that do encounter problems warrant careful consideration. These issues can be broadly categorized into two main groups: early-stage complications, which occur during or shortly after the surgical placement, and late-stage complications, which can develop months or even years down the line.
## Understanding Early vs. Late-Stage Complications
Immediate and Early-Stage Issues
Long-Term and Late-Stage Complications
Late-stage complications can surface after the implant has successfully integrated with the bone and the final crown has been placed. These issues are more often related to long-term maintenance, patient habits, or mechanical wear and tear. The most significant and prevalent late-stage complication is peri-implantitis. This is an inflammatory condition affecting the gum and bone tissue surrounding the implant, akin to gum disease around a natural tooth. If left untreated, it can lead to progressive bone loss and the eventual failure of the implant. Mechanical failures can also occur over time. These include the loosening of the abutment screw that connects the crown to the implant, or, more rarely, the fracture of the implant or its components. These mechanical issues are often associated with excessive biting forces, such as those from teeth grinding (bruxism).
## A Detailed Look at Common Dental Implant Complications
Peri-Implantitis: The Primary Threat to Implant Longevity
Peri-implantitis is the leading cause of late implant failure. It begins as peri-mucositis, a reversible inflammation of the gums around the implant, characterized by redness and bleeding upon brushing. This is caused by plaque biofilm accumulation due to inadequate oral hygiene. If this plaque is not removed, it can progress to peri-implantitis, where the inflammation extends deeper, causing the destruction of the supporting bone. Symptoms include bleeding gums, deep pockets forming around the implant, pus discharge, and eventually, the implant becoming loose. Prevention is centered on meticulous daily oral hygiene and regular professional cleanings. Treatment for established peri-implantitis can range from non-surgical debridement to surgical procedures aimed at decontaminating the implant surface and, in some cases, bone grafting to repair the lost bone.
Failure of Osseointegration
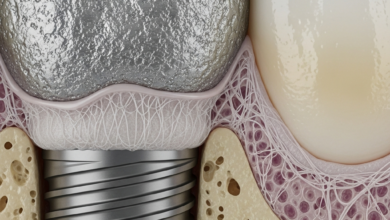
Osseointegration is the remarkable biological process where the jawbone fuses directly with the titanium surface of the dental implant, creating a strong and stable foundation. If this fusion fails to occur, the implant will not be stable enough to support a prosthetic tooth. This failure can be caused by several factors. Insufficient bone quantity or quality is a primary cause, which is why bone grafting is sometimes a necessary preliminary step. Certain systemic health conditions, particularly uncontrolled diabetes, can impair healing and hinder osseointegration. Smoking is another major risk factor, as it constricts blood vessels and reduces the body’s ability to heal. Premature loading, or placing biting forces on the implant before it has fully integrated, can also disrupt the healing process and lead to failure.
| Complication | Category | Typical Onset | Key Symptoms | Primary Cause(s) |
|---|---|---|---|---|
| Peri-implantitis | Biological | Late-Stage (Months to Years) | Bleeding gums, pus, bone loss, implant mobility | Poor oral hygiene, smoking, genetic predisposition |
| Osseointegration Failure | Biological | Early-Stage (First 3-6 Months) | Implant mobility, pain upon pressure, lack of stability | Poor bone quality, smoking, uncontrolled diabetes, premature loading |
| Nerve Damage | Surgical | Immediate | Numbness, tingling, or pain in lip, chin, or tongue | Implant placement too close to a nerve canal |
| Abutment Screw Loosening | Mechanical | Late-Stage | Crown feels loose or wobbly | Excessive bite forces (bruxism), improper fit |
| Sinus Perforation | Surgical | Immediate | Sinus pressure, nasal congestion, nosebleed | Implant extends into the maxillary sinus cavity |
## Prevention and Proactive Management
The Crucial Role of Patient Diligence
Once the implant is in place, its long-term health is largely in the patient’s hands. Meticulous oral hygiene is non-negotiable. This means brushing twice daily, as well as using specialized tools like water flossers, interdental brushes, or implant-specific floss to clean around the implant abutment. Regular professional check-ups and cleanings, typically every six months, are essential for early detection of any issues like peri-mucositis before they can escalate. Lifestyle choices also play a significant role. Quitting smoking dramatically increases the success rate, and managing systemic conditions like diabetes is vital for maintaining gum and bone health.
The Importance of Expert Planning and Execution
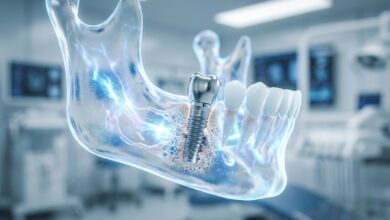
The prevention of complications begins long before the surgery. A thorough evaluation, including 3D imaging with a Cone Beam Computed Tomography (CBCT) scanner, allows the surgeon to precisely plan the implant’s position, avoiding critical structures like nerves and sinuses while ensuring it is placed in the densest available bone. Choosing an experienced surgeon who uses high-quality materials and adheres to strict sterile protocols significantly minimizes surgical risks. Understanding these potential issues is a crucial part of the consent process, and a detailed discussion of all dental implant risks should occur before any procedure. The design of the final restoration must also be considered, as a well-designed crown will distribute biting forces evenly and be easy for the patient to clean around.
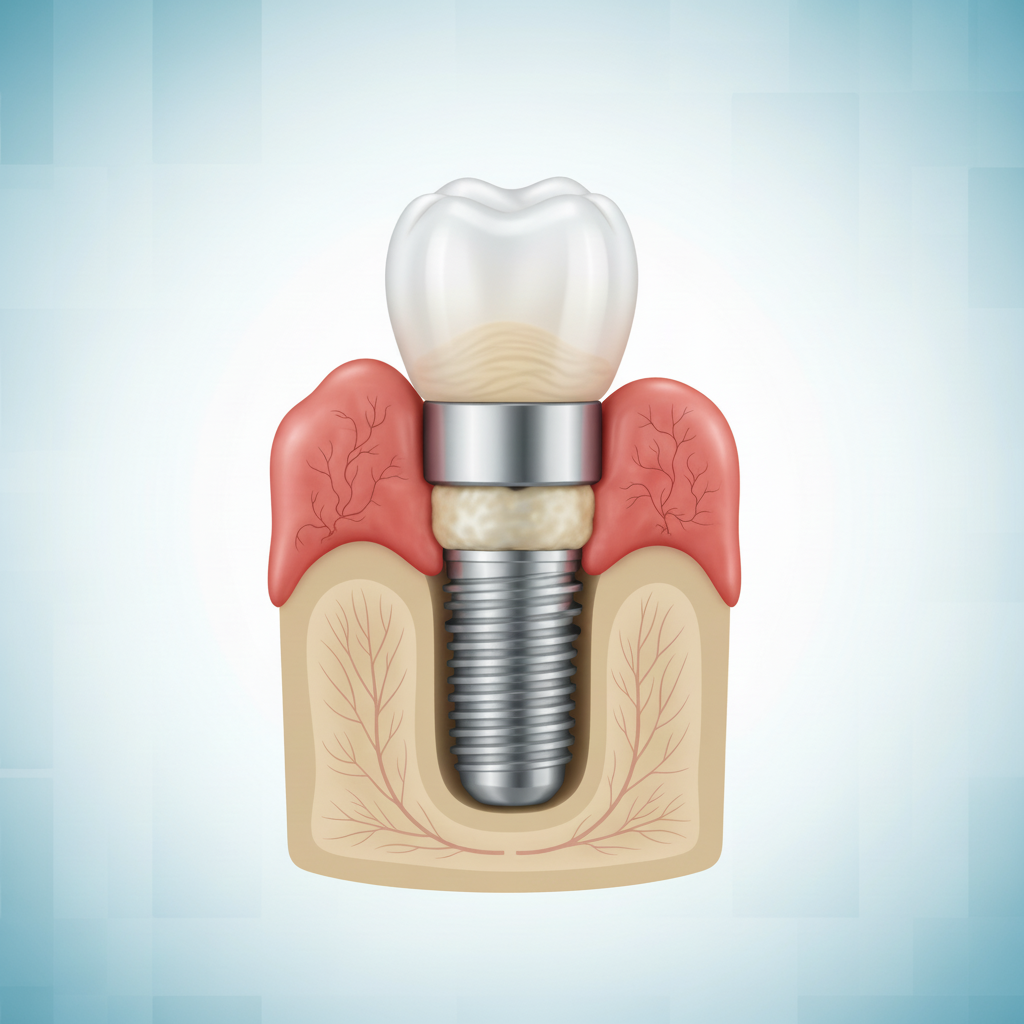
Should a complication arise, early intervention is key. A loose abutment screw can often be simply tightened. Early-stage peri-mucositis can typically be reversed with professional cleaning and improved home care. For more advanced problems like peri-implantitis, treatment becomes more complex and may involve surgical procedures to clean the implant surface and regenerate lost bone. In severe cases of implant failure or advanced bone loss, the implant may need to be removed. After a healing period, it is often possible to place a new implant, sometimes with bone grafting to rebuild the site. A comprehensive review of dental implant complications published by the National Center for Biotechnology Information details the various diagnostic and therapeutic approaches used by clinicians to manage these complex situations. This highlights the importance of seeking care from a team well-versed in both placing and maintaining dental implants. Ultimately, the high success rate of dental implants is achieved not because complications never happen, but because they can be successfully prevented and managed with expertise, technology, and patient cooperation.