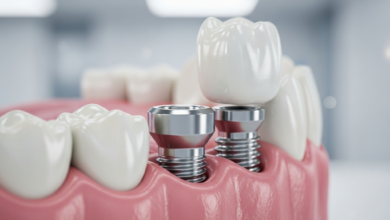
Dental Implants for Seniors Guide

Dental Implants for Seniors Guide. As we age, maintaining oral health becomes increasingly crucial for overall well-being, nutrition, and quality of life. Tooth loss, a common issue among older adults, can significantly impact one’s ability to eat, speak, and smile with confidence. For decades, traditional dentures were the primary solution. However, modern dentistry offers a superior, permanent alternative: dental implants. This advanced treatment provides a stable, functional, and aesthetically pleasing replacement for missing teeth, and contrary to some beliefs, age is rarely a barrier to a successful outcome. Implants represent a transformative investment in health, restoring not just a smile, but the full function of a natural bite.
Understanding How Dental Implants Work
Dental implants are a sophisticated solution designed to mimic the structure and function of natural teeth. They are surgically placed into the jawbone, where they act as artificial tooth roots, providing a strong foundation for replacement teeth. Understanding the components and the biological process behind their success is key to appreciating their value, especially for senior patients.
The Three Core Components of a Dental Implant
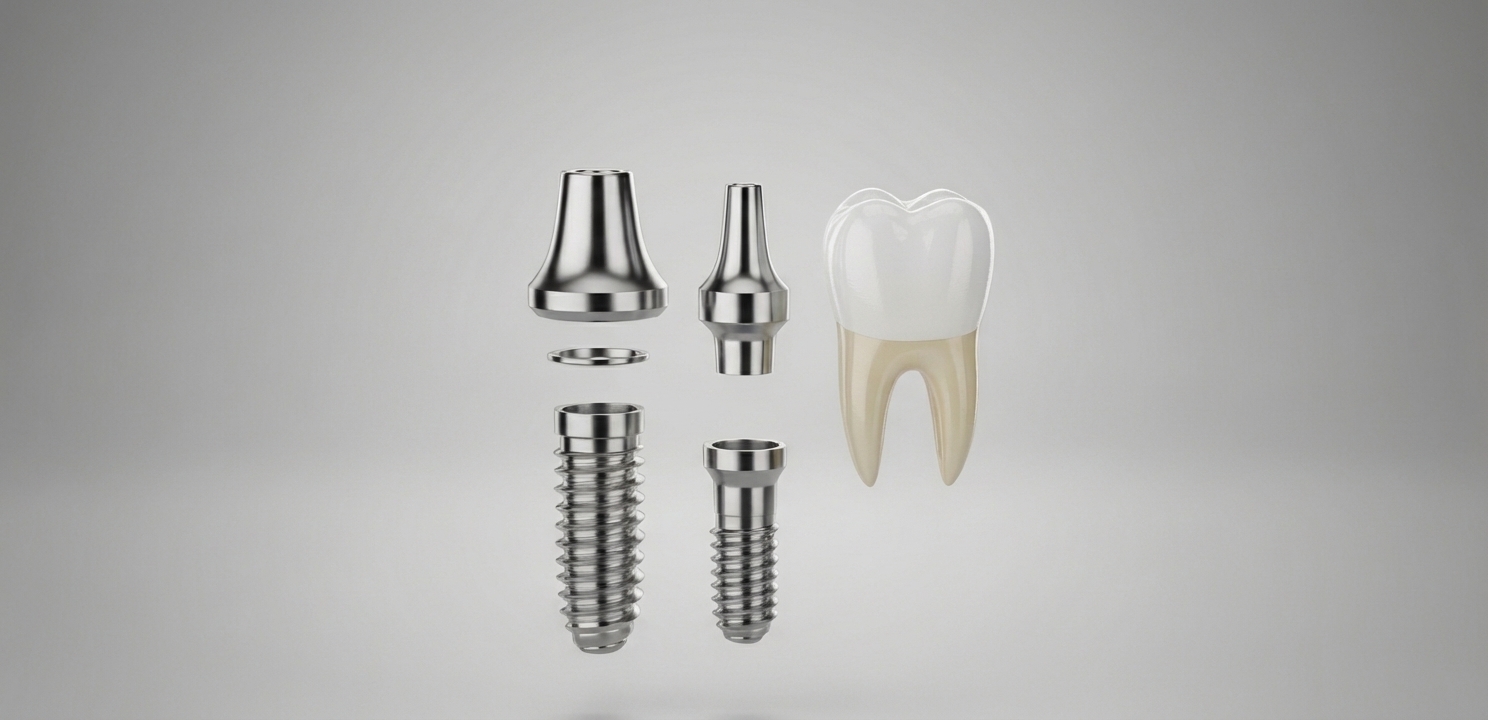
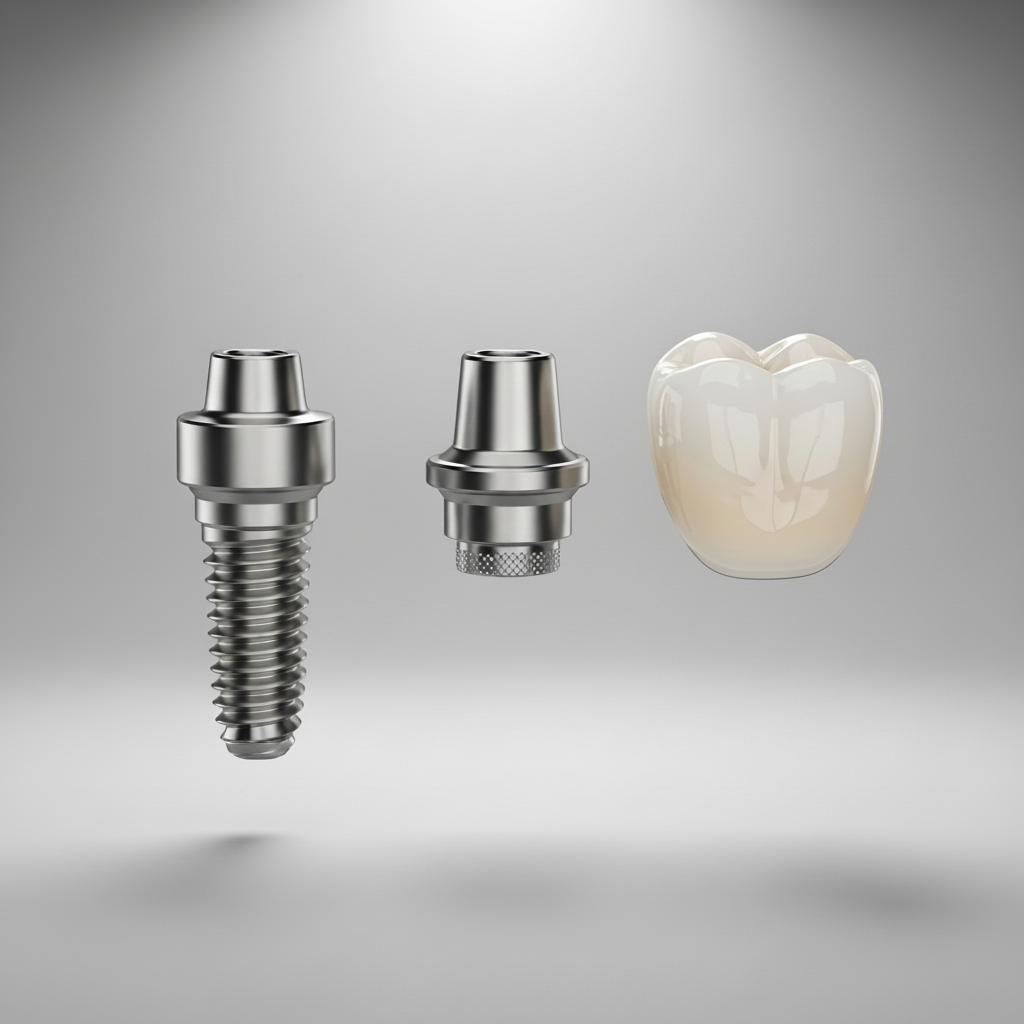
A complete dental implant restoration consists of three main parts working in harmony:
- The Implant Fixture: This is a small, screw-like post typically made from biocompatible titanium. It is surgically inserted directly into the jawbone in the space left by a missing tooth. This titanium post serves as the replacement for the natural tooth root.
- The Abutment: After the implant fixture has fully integrated with the bone, a connector piece called an abutment is attached. The abutment protrudes just above the gum line and acts as the bridge between the implant fixture and the final crown.
- The Crown: This is the visible, tooth-shaped part of the restoration. The crown is custom-made to match the color, shape, and size of the patient’s surrounding natural teeth, ensuring a seamless and natural-looking result. It is securely attached to the abutment to complete the restoration.
The Osseointegration Process Explained
The magic behind the stability of dental implants lies in a biological process called osseointegration. This term describes the remarkable ability of living bone to fuse directly with the surface of the biocompatible titanium implant. When the fixture is placed, the bone begins to grow onto and into its specially treated surface. This fusion creates an incredibly strong and durable bond, effectively making the implant a permanent part of the jaw. This process typically takes three to six months to complete. The high success rate of this fusion is well-documented, even in older populations. Research shows that the survival of dental implants in the elderly is comparable to that in younger patients, confirming that a healthy patient, regardless of age, can achieve successful osseointegration.
Key Benefits of Dental Implants for Seniors
For seniors, the advantages of choosing dental implants over other tooth replacement options extend far beyond simple aesthetics. They offer profound improvements in health, function, and overall quality of life.
Restored Function and Improved Nutrition
One of the most significant challenges for seniors with missing teeth or ill-fitting dentures is difficulty chewing. This often leads to a restricted diet of soft, processed foods, which can result in poor nutrition. Dental implants restore full chewing power, allowing individuals to enjoy a diverse and balanced diet rich in fruits, vegetables, and proteins. This improved nutritional intake is directly linked to better overall physical health and vitality.
Preventing Bone Loss and Preserving Facial Structure
When a tooth is lost, the jawbone in that area no longer receives the stimulation it needs from chewing forces. As a result, the bone begins to deteriorate, or resorb. This bone loss can lead to a sunken facial appearance, making a person look older than they are. Dental implants are the only tooth replacement solution that stimulates the jawbone just like natural tooth roots, preventing bone resorption and preserving the natural contours of the face and jaw.
| Feature | Dental Implants | Traditional Dentures |
|---|---|---|
| Stability | Permanently fused with the jawbone; no slipping or movement. | Rest on the gums; can slip, click, or fall out while speaking or eating. |
| Bone Health | Stimulates the jawbone, preventing bone loss. | Does not stimulate the bone; can accelerate jawbone deterioration over time. |
| Comfort | Feel and function like natural teeth; no gum irritation. | Can cause sore spots, gum irritation, and discomfort from rubbing. |
| Maintenance | Care for them like natural teeth (brushing, flossing). | Require removal for cleaning, soaking, and use of special adhesives. |
| Dietary Freedom | No restrictions; can eat hard, sticky, and chewy foods. | Diet is often restricted to softer foods; difficult to eat certain items. |
| Longevity | Can last a lifetime with proper care. A long-term investment. | Need to be relined or replaced every 5-10 years as the jaw changes shape. |
Are Dental Implants for Seniors a Safe Option?
A primary concern for many older adults is whether they are suitable candidates for a surgical procedure. The truth is that candidacy for dental implants is determined more by a person’s overall health than by their chronological age. A healthy individual in their 70s, 80s, or even 90s can be a better candidate than a younger person with significant unmanaged health issues.
Health Conditions and Candidacy
A thorough medical evaluation is the first step. Chronic conditions such as well-managed diabetes, heart disease, or osteoporosis are not automatic disqualifiers. The key is that these conditions are under control and stable. The implant specialist will work closely with the patient’s primary physician to ensure the procedure can be performed safely. Uncontrolled diabetes can impair healing, and certain medications for osteoporosis can affect the jawbone, so a comprehensive health history review is essential for planning a successful treatment.
The Importance of Bone Density
Sufficient jawbone density and volume are necessary to securely anchor the implant. Long-term tooth loss can lead to significant bone resorption, which might be a concern for some senior patients. However, this does not rule out implants. Advanced imaging techniques like a Cone Beam Computed Tomography (CBCT) scan allow the surgeon to precisely measure the available bone. If bone volume is inadequate, procedures such as a bone graft can be performed to augment the area, creating a solid foundation for the future implant.
The Dental Implant Procedure: A Step-by-Step Overview
The process of receiving dental implants is a multi-stage journey that is carefully planned and executed. Understanding these steps can help alleviate any anxiety about the treatment.
- Initial Consultation and Planning: This crucial first step involves a comprehensive oral examination, a review of medical history, and advanced 3D imaging. This allows the dental team to assess bone quality, determine the precise placement for the implant(s), and create a detailed, personalized treatment plan.
- Implant Placement Surgery: This is a minor surgical procedure, typically performed in the dental office with local anesthesia. The surgeon makes a small incision in the gum tissue to access the bone, prepares the site, and carefully places the titanium implant fixture into the jaw. The site is then closed with a few stitches.
- Healing and Osseointegration: Following placement, a healing period of several months is required. During this time, the process of osseointegration occurs as the jawbone fuses with the implant. A temporary tooth replacement may be worn during this phase.
- Abutment and Crown Placement: Once the implant is fully integrated, the abutment is attached. After the gums have healed around the abutment, the final, custom-made crown is secured in place, completing the process and restoring a fully functional tooth. For patients needing multiple teeth replaced, this may involve a bridge or even a comprehensive full mouth restoration.
Recovery and Aftercare for Senior Patients
The recovery from implant surgery is generally well-tolerated. Post-operative care is straightforward and essential for long-term success.
Managing Post-Procedure Discomfort
Some minor swelling, bruising, and discomfort are normal after the placement procedure. These symptoms are typically manageable with over-the-counter pain relievers and the use of cold packs on the outside of the cheek. A diet of soft foods is recommended for the first few days to avoid putting pressure on the surgical site. The dental team provides detailed post-operative instructions to ensure a smooth and comfortable recovery.
Long-Term Oral Hygiene and Maintenance
Dental implants are resistant to decay, but the surrounding gum tissue is not. Therefore, maintaining excellent oral hygiene is vital. This includes brushing twice daily, flossing around the implant (a water flosser can be a very effective tool), and attending regular dental check-ups and cleanings. With proper care, dental implants can last a lifetime, providing a permanent and reliable solution to tooth loss, allowing seniors to live their later years with renewed health, confidence, and a beautiful smile.