How Long Do Dental Implants Last
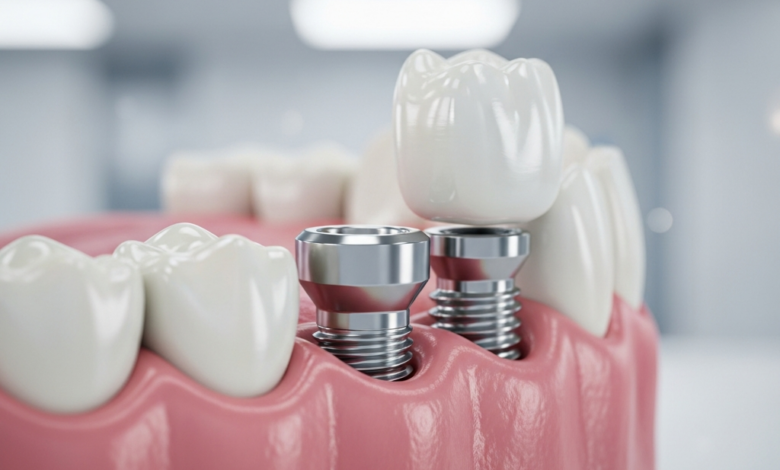
How Long Do Dental Implants Last is one of the most important questions patients ask when considering this life-changing tooth replacement solution. Unlike other options such as bridges or dentures, dental implants are designed to be a permanent and durable foundation for new teeth. With proper care and under ideal conditions, a dental implant can last a lifetime. However, the longevity of the complete restoration involves understanding the different components and the various factors that influence their success over the years. A dental implant is not just a single piece; it’s a system composed of the implant post, the abutment, and the final restoration (the crown). Each part has a different role and potentially a different lifespan, all of which contribute to the overall answer.

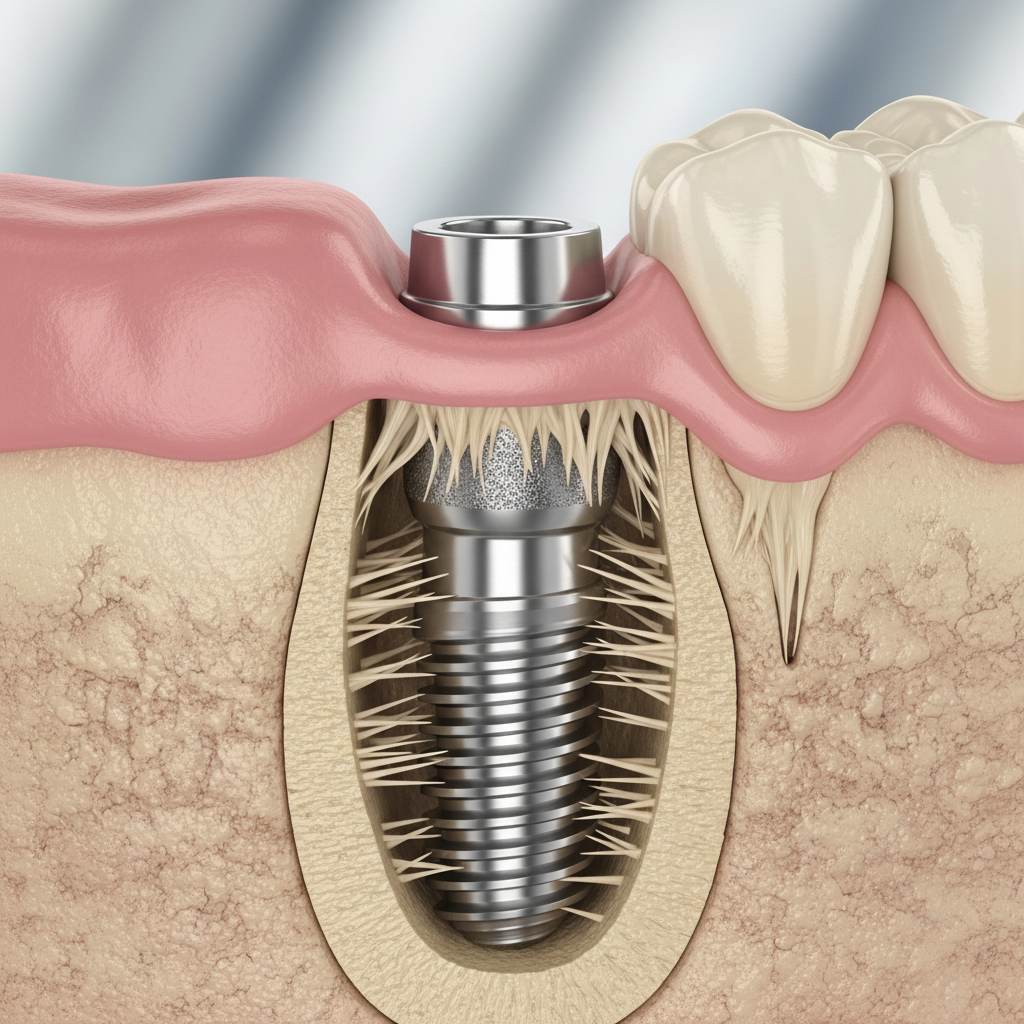
The implant itself is a small, screw-like post, typically made of biocompatible titanium, which is surgically placed into the jawbone. This post acts as a replacement for the natural tooth root. The remarkable success of this component lies in a process called osseointegration, where the jawbone grows around and fuses directly with the titanium post. This creates an incredibly strong and stable anchor. Because this fusion makes the implant a part of your jaw, the post itself is not subject to decay and, if the surrounding bone remains healthy, it can genuinely last for the rest of a person’s life. It is the foundation upon which everything else is built, and its permanence is the primary advantage of implant-based restorations.
The Lifespan of Different Implant Components
While the titanium post is designed for permanence, the components attached to it are subject to the daily wear and tear of chewing and biting. It’s crucial to differentiate between the implant post and the dental crown that sits on top of it. This distinction is key to understanding the long-term maintenance and potential costs associated with dental implants.
The Implant Post (The Fixture)
As mentioned, the implant post that fuses with the jawbone is the core of the system. Its longevity is exceptionally high. The primary threat to the implant post is not wear and tear but a condition similar to gum disease called peri-implantitis. This is an inflammatory condition affecting the gum and bone tissue surrounding an implant. If plaque and bacteria are allowed to accumulate, it can lead to inflammation, gum recession, and eventually, bone loss around the implant. Severe bone loss can compromise the implant’s stability, leading to failure. Therefore, the lifetime potential of the implant post is directly tied to excellent oral hygiene and regular professional dental care to prevent peri-implantitis.
The Abutment and Crown (The Restoration)
The abutment is a connector piece that is attached to the implant post and protrudes through the gum line. The final restoration, which is typically a ceramic or porcelain crown, is then cemented or screwed onto this abutment. The crown is the part of the implant system that looks and functions like a natural tooth. Because it is exposed to the forces of biting and chewing, it is the most likely component to require replacement over time. On average, a high-quality dental crown can last between 10 to 15 years, but this can vary significantly. Some crowns can last much longer, upwards of 20 or 25 years, especially with meticulous care and if the patient does not have habits like teeth grinding (bruxism).
How Long Do Dental Implants Last: Factors Influencing Longevity
The success and lifespan of a dental implant are not guaranteed; they are heavily influenced by a combination of biological, mechanical, and lifestyle factors. A patient’s commitment to aftercare plays the most significant role in ensuring the implant serves them well for decades to come. Understanding these factors helps patients take an active role in protecting their investment in their oral health.
| Influencing Factor | Impact on Implant Lifespan |
|---|---|
| Oral Hygiene | Critical. Poor hygiene leads to peri-implantitis, the leading cause of late-stage implant failure. Daily brushing, flossing, and regular check-ups are non-negotiable for long-term success. |
| Smoking & Tobacco Use | Highly Negative. Smoking restricts blood flow, impairs the healing process of osseointegration, and significantly increases the risk of infection and peri-implantitis. |
| Jawbone Density & Volume | Fundamental. Sufficient, healthy bone is required for the initial fusion (osseointegration). Bone grafting may be needed to build up the site before placement, ensuring a stable foundation. |
| Dentist’s Skill & Experience | Very High. The precise placement, angle, and depth of the implant are crucial for long-term stability and function. Choosing an experienced implantologist is essential. |
| Overall Health | Significant. Uncontrolled conditions like diabetes or osteoporosis can interfere with healing and bone health, potentially increasing the risk of complications. |
| Location in the Mouth | Moderate. Implants in the back of the mouth endure greater chewing forces, which can lead to more wear on the crown over time compared to front teeth. |
The Critical Role of Maintenance and Hygiene
Without question, the most important variable within the patient’s control is their commitment to oral hygiene. An implant cannot get a cavity, but it can fail due to gum and bone disease. Consistent and thorough dental implant maintenance is the single most important factor in its longevity. This includes brushing twice a day, flossing daily (using special implant-friendly floss or a water flosser is highly recommended to clean around the abutment), and attending all scheduled professional cleanings and check-ups. During these visits, the dentist and hygienist can assess the health of the gums and bone around the implant and perform cleanings that remove hardened plaque (tartar) that regular brushing cannot.
Lifestyle Choices and Overall Health
Lifestyle habits have a profound impact. As noted, smoking is one of the biggest risk factors for implant failure. The chemicals in tobacco smoke can damage gum tissue and bone cells, making the area around the implant more susceptible to infection and failure. Furthermore, certain systemic health conditions can affect the body’s ability to heal and maintain bone density. Patients with uncontrolled diabetes, for example, may experience slower healing and a higher risk of infection. It is vital to manage any chronic health conditions and to inform your dental surgeon of your complete medical history before beginning treatment.
Long-Term Success Rates and Protecting Your Investment
Dental implants have one of the highest success rates of any dental procedure. The long-term viability is well-documented in clinical research. Extensive studies have followed patients for many years to track how well implants perform over time. Scientific literature consistently reports long-term survival rates of 90-95% or even higher at the 10-year mark, with many lasting much longer. This data underscores that when placed correctly in a healthy candidate who maintains them properly, dental implants are an incredibly reliable and predictable solution for tooth loss.
Protecting this investment means treating the implant with the same care and respect as a natural tooth. Avoid using your teeth—implant or natural—as tools to open packages or bite on non-food items like ice, pens, or fingernails. If you suffer from bruxism (teeth grinding), your dentist will strongly recommend a custom-fitted nightguard. This appliance protects the ceramic crown from the immense pressure of grinding, which can cause it to chip, crack, or wear down prematurely. By adopting these protective habits and committing to a diligent oral care routine, you are creating the best possible environment for your dental implant to last a lifetime, providing a stable, confident, and beautiful smile for many years to come.