Bone Grafting for Dental Implants Guide

The primary categories of graft materials are:
- Autografts: This involves harvesting bone from another part of the patient’s own body, such as the chin, the back of the jaw, or even the hip. It is often considered the gold standard because it contains the patient’s own living bone cells, eliminating any risk of rejection.
- Allografts: This material is sourced from a human cadaver donor. The bone is rigorously screened, sterilized, and processed in a tissue bank to ensure it is safe for transplantation. It acts as an excellent scaffold for the patient’s bone to grow into.
- Xenografts: This graft material is derived from a non-human source, most commonly bovine (cow) bone. The bone is processed to remove all organic material, leaving only the mineral framework, which is very similar to human bone and serves as a highly effective scaffold for new bone formation.
- Alloplasts: These are synthetic, biocompatible materials created in a laboratory. They are typically made from substances like hydroxyapatite or tricalcium phosphate, which are minerals naturally found in human bone. Alloplasts provide a framework that the body can resorb and replace with its own bone.
Comparison of Bone Grafting Materials
| Graft Type | Source | Primary Advantage | Primary Disadvantage |
|---|---|---|---|
| Autograft | Patient’s own body (e.g., chin, hip) | Contains live cells; zero risk of rejection. | Requires a second surgical site for harvesting. |
| Allograft | Human donor (tissue bank) | No second surgical site; readily available. | Sterilized material lacks live cells; minimal risk of disease transmission. |
| Xenograft | Animal source (typically bovine) | Highly effective scaffold; abundant supply. | Cultural or personal objections; very slow resorption rate. |
| Alloplast | Synthetic (laboratory-made) | No risk of disease transmission; unlimited supply. | Variable effectiveness compared to natural bone sources. |
The Bone Grafting Procedure and Recovery Timeline
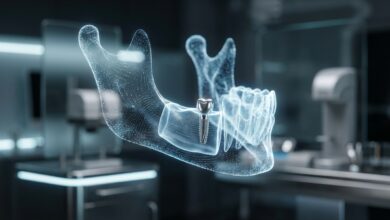
The bone grafting procedure is a precise surgical technique performed by a skilled oral surgeon or periodontist. It begins with a thorough evaluation, including 3D imaging like a Cone Beam Computed Tomography (CBCT) scan, to accurately assess the bone’s height, width, and density.
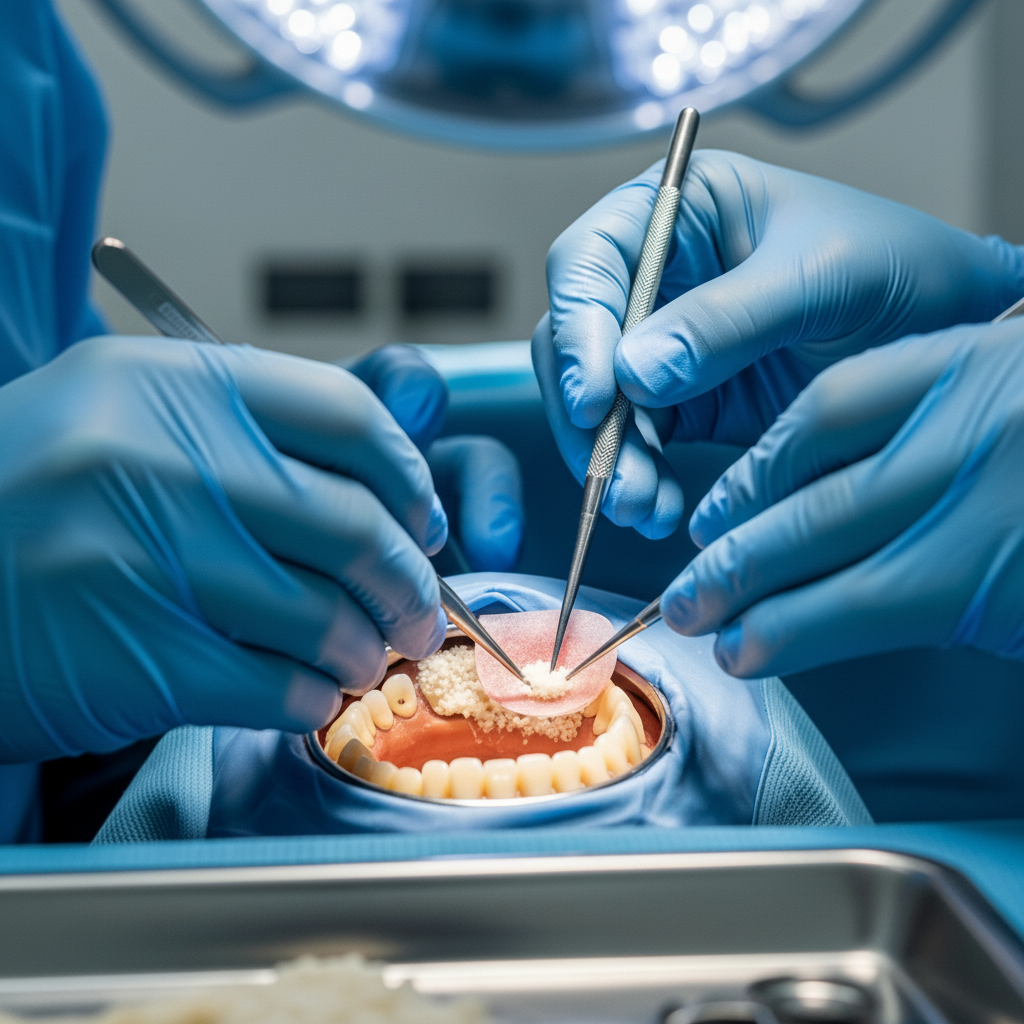
The surgery itself is typically performed under local anesthesia. The surgeon makes a small incision in the gum tissue to expose the underlying jawbone. The chosen graft material is then carefully placed in the area requiring augmentation. Often, a special biocompatible membrane is placed over the graft to protect it and to guide the growth of new bone tissue, preventing the faster-growing gum tissue from interfering. The incision is then closed with sutures.
Recovery from a bone graft is a critical phase. Patients are provided with detailed aftercare instructions to manage swelling and minor discomfort, which can be controlled with prescribed or over-the-counter pain relievers. A diet of soft foods is recommended for the initial period to avoid putting pressure on the surgical site. Proper oral hygiene is vital, though patients will be advised to be very gentle around the treated area. The most important part of recovery is time. The body needs several months for the graft to mature and integrate fully with the existing jawbone. The timeline for healing can range from three to nine months, after which the site is re-evaluated to confirm it is ready for dental implant placement for bone loss patients. Scientific studies have shown that various grafting techniques can successfully regenerate bone, enabling predictable implant placement. According to a review published in the National Center for Biotechnology Information, both autogenous bone and bone substitutes are effective in augmenting the jawbone for future implant support. Following the surgeon’s instructions precisely during this healing period is paramount to achieving a successful outcome and creating a solid, lasting foundation for a new smile.
Bone Grafting for Dental Implants Guide to achieving a strong foundation for a lasting smile. For many individuals seeking the permanence and functionality of dental implants, the journey begins not with the implant itself, but with a crucial preparatory step: bone grafting. A dental implant, which acts as an artificial tooth root, requires a sufficient amount of healthy jawbone to anchor it securely. When the jawbone lacks the necessary volume or density, a bone grafting procedure becomes essential to build up the bone, creating a stable and durable base for the future implant. This process is fundamental to the long-term success of the implant and the overall restoration of a healthy, functional bite.
Understanding why bone volume diminishes is the first step in appreciating the need for this procedure. The jawbone maintains its mass and density through the stimulation it receives from tooth roots during daily activities like chewing. When a tooth is lost, that stimulation ceases. The body, in its efficiency, begins to resorb the bone material in that area, as it no longer perceives a need for it. This process, known as bone atrophy, can be surprisingly rapid, with significant bone loss occurring within the first year after a tooth is extracted. Other causes of jawbone deterioration include advanced periodontal (gum) disease, infections, facial trauma, or developmental defects. Without intervention, this loss of bone can not only prevent the placement of dental implants but also alter facial structure, leading to a sunken appearance.
Why Is a Bone Graft Necessary for a Dental Implant?
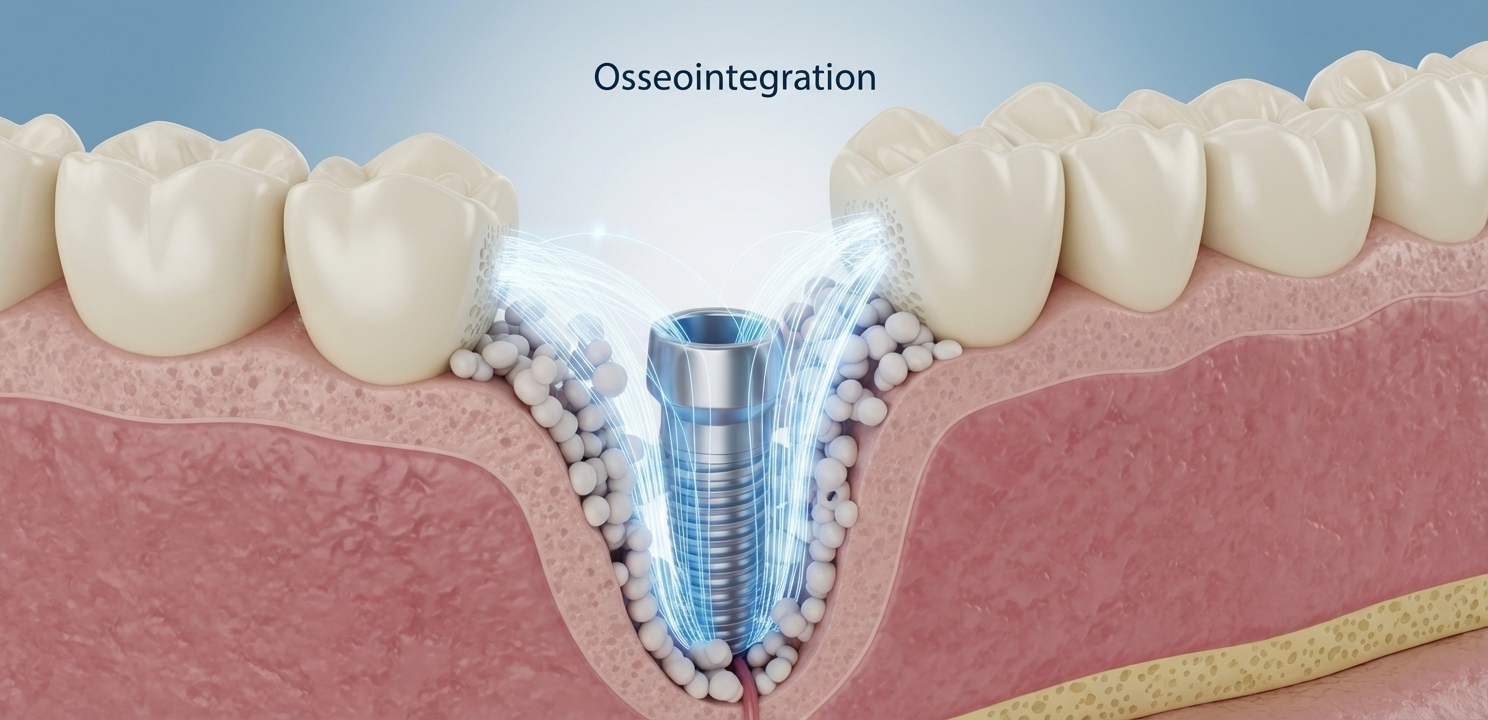
The success of a dental implant is measured by its ability to integrate with the surrounding bone in a process called osseointegration. During this biological process, the jawbone grows into and fuses with the titanium surface of the implant, creating an incredibly strong and stable connection that mimics a natural tooth root. For osseointegration to occur successfully, the implant must be completely enveloped by a sufficient quantity of healthy bone. If the jaw ridge is too thin, too short, or too soft, it cannot provide the initial stability required for the implant to heal and integrate.
Attempting to place an implant in inadequate bone is a leading cause of implant failure. The implant may fail to integrate, become loose over time, or even lead to complications such as nerve damage or sinus perforation. Therefore, Bone Grafting for Dental Implants is not merely an optional enhancement; it is a foundational requirement for candidates with compromised jawbone structure. The graft serves as a scaffold, encouraging the patient’s own body to generate new bone tissue in the deficient area. Over several months, the grafted material is gradually replaced by new, living bone, creating the ideal dimensions and density needed to support an implant securely for decades to come.
Exploring the Different Types of Bone Graft Materials
Modern dentistry utilizes several types of bone graft materials, each with specific characteristics and applications. The choice of material depends on the size of the defect, the location in the jaw, and the surgeon’s recommendation. The goal is always to provide a safe and effective framework for new bone growth.