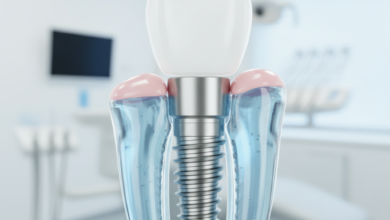
Dental Implants for Bone Loss Patients
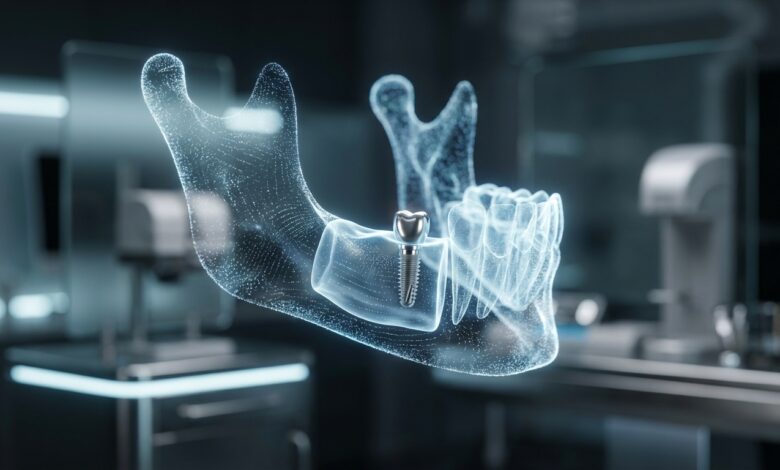
Dental Implants for Bone Loss Patients are no longer a contradiction in terms. For years, individuals suffering from significant jawbone deterioration were often told they were not candidates for dental implants, the gold standard in tooth replacement. This left them with less stable and often uncomfortable options like dentures. However, advancements in dental technology and surgical techniques have dramatically changed the landscape. Today, having insufficient bone volume is not an endpoint but rather a challenge that experienced implantologists can overcome with sophisticated procedures, restoring not just smiles, but the very foundation of oral health.
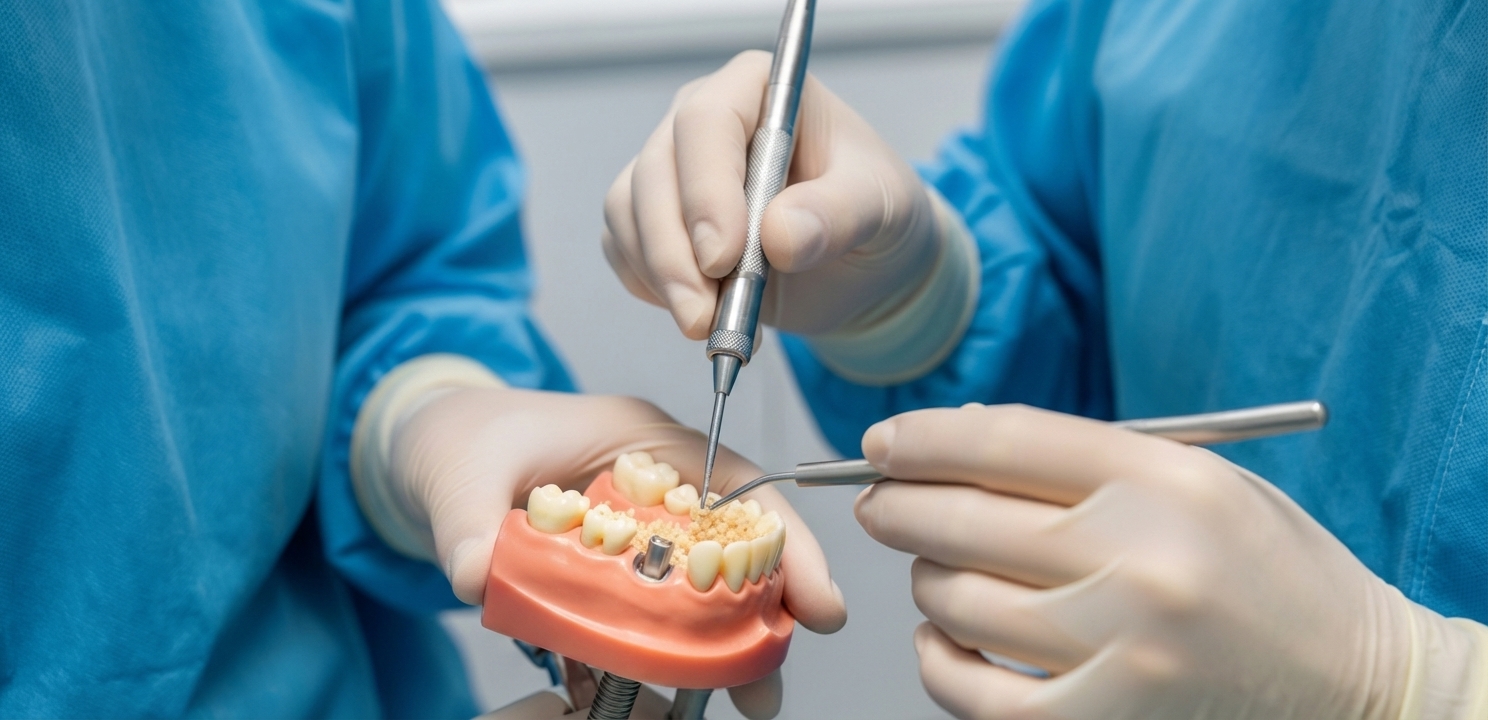
Understanding the connection between missing teeth and bone loss is the first step. The jawbone, much like a muscle, requires constant stimulation to maintain its density and volume. The roots of your natural teeth provide this vital stimulation every time you chew. When a tooth is lost, that stimulation ceases. The body, in its efficiency, begins to resorb the bone material in that area, viewing it as no longer necessary. This process, known as jawbone atrophy, can lead to a loss of up to 25% of bone width in the first year after tooth loss and continues over time, leading to significant structural changes in the face and jaw.
Understanding Jawbone Loss and Its Impact on Dental Health
Jawbone deterioration is a silent process that can have profound consequences for your oral and overall health. It’s not merely a cosmetic issue; it affects your ability to eat, speak, and support remaining teeth. A strong, dense jawbone is the critical foundation required for the long-term success of dental implants, which need to fuse directly with the bone in a process called osseointegration. Without adequate bone, an implant has nothing to anchor to, making the procedure impossible without preliminary intervention.
Why Does Jawbone Deterioration Occur?
Several factors can initiate or accelerate the loss of jawbone mass. The most common cause is tooth extraction or loss. Without the tooth root to stimulate the alveolar bone, the bone begins to shrink. Other significant causes include:
- Periodontal (Gum) Disease: Chronic gum infections can destroy the ligaments and bone that support the teeth, leading to widespread bone loss even before teeth are lost.
- Prolonged Denture Wear: Traditional dentures rest on the gum tissue. Over time, the constant pressure on the gums can accelerate the resorption of the underlying bone, leading to a poor fit and the characteristic “sunken” facial appearance.
- Trauma or Injury: A significant injury to the jaw can damage the bone, leading to its resorption in the affected area.
- Developmental Abnormalities or Tumors: In some cases, congenital conditions or the surgical removal of a tumor can result in significant bone defects.
The Consequences of Ignoring Bone Atrophy
Allowing jawbone atrophy to progress can lead to a cascade of dental problems. The most visible effect is a change in facial aesthetics, including a collapsed facial profile, thinning lips, and more pronounced wrinkles around the mouth. Functionally, it becomes increasingly difficult to chew food properly, which can lead to nutritional deficiencies. Remaining teeth may shift or drift into the empty spaces, causing bite problems and further complicating future restorative work. For dental implant candidates, the most direct consequence is being disqualified for the procedure due to an unstable foundation.
Advanced Solutions: How Dental Implants for Bone Loss Are Possible
The solution to insufficient bone for dental implants lies in rebuilding this crucial foundation. Modern implant dentistry focuses on regenerative procedures that augment the existing jawbone, creating the necessary height, width, and density to securely support an implant. The cornerstone of this approach is bone grafting. This surgical procedure involves adding bone, or a bone-like material, to the deficient area of the jaw. Over several months, the body uses this grafted material as a scaffold, eventually replacing it with new, strong, and living bone, fully integrated into the jaw.
The Crucial Role of Bone Grafting in Implant Dentistry
A bone graft is not just a placeholder; it is an active biological process. The material placed stimulates the body’s own bone-generating cells to migrate to the area and begin depositing new bone tissue. The goal is to create a site that is structurally sound enough to withstand the forces of chewing transmitted through a dental implant. A successful graft ensures that the subsequent implant placement has the highest possible chance of successful osseointegration, which is the biological fusion of the titanium implant to the surrounding bone. This fusion is what gives dental implants their incredible stability and longevity, making them function just like natural teeth.
Exploring Bone Grafting Techniques for Implant Success
There is no one-size-fits-all approach to bone grafting. The specific technique and material used depend on the location and extent of the bone loss. An implant specialist will use 3D imaging, like a Cone Beam Computed Tomography (CBCT) scan, to precisely evaluate the bone volume and plan the most effective grafting strategy. The materials used fall into several main categories, each with distinct properties and applications.
Comparison of Common Bone Grafting Materials
Choosing the right graft material is essential for a predictable and successful outcome. The decision is based on the patient’s specific needs, the size of the defect, and the dentist’s clinical judgment. Below is a comparison of the most commonly used materials in dental implantology.
| Graft Type | Source | Key Advantages | Key Considerations |
|---|---|---|---|
| Autograft | Patient’s Own Body (e.g., chin, hip) | The “gold standard.” Contains live bone cells, promotes rapid healing, and has no risk of immune rejection. | Requires a second surgical site to harvest the bone, which can increase discomfort and recovery time. |
| Allograft | Donated Human Tissue (from a tissue bank) | Eliminates the need for a second surgical site. Readily available in various shapes and sizes. | Material is sterile and processed for safety, but does not contain live cells, leading to a slightly slower integration process. |
| Xenograft | Animal Source (typically bovine/cow) | Highly biocompatible and acts as an excellent, slow-resorbing scaffold for new bone growth. Widely studied and used. | The material itself does not turn into host bone but provides a framework for the patient’s bone to grow into. |
| Alloplast | Synthetic Materials (e.g., hydroxyapatite) | Completely synthetic, eliminating any risk of disease transmission. Unlimited supply and biocompatible. | Primarily serves as a scaffold (osteoconductive) and lacks the biological growth factors found in natural bone. |
The Step-by-Step Process: From Consultation to Final Crown
The journey to receiving dental implants with a bone graft is a multi-stage process that requires patience but yields life-changing results.
- Consultation and Planning: This begins with a comprehensive examination and CBCT scan to assess the bone quality and quantity. A detailed treatment plan is created.
- The Bone Grafting Procedure: The specialist surgically places the chosen graft material at the deficient site. A protective membrane is often placed over the graft to guide bone regeneration and prevent soft tissue from growing into the space.
- Healing and Maturation: This is a critical waiting period of 4 to 9 months. During this time, the body’s natural healing processes transform the graft material into solid, mature bone capable of supporting an implant.
- Implant Placement: Once the jawbone is confirmed to be sufficiently healed and dense, the titanium implant post is surgically inserted into the bone.
- Osseointegration: A second healing phase of 3 to 6 months begins, during which the jawbone fuses directly onto the surface of the implant. This process of osseointegration is fundamental to the stability and success of the implant.
- Final Restoration: After osseointegration is complete, an abutment is attached to the implant, and the final, custom-made crown is secured, completing the restoration.
Are There Alternatives to Extensive Bone Grafting?
In some specific cases of severe bone loss, particularly in the upper jaw, alternative techniques can be employed to minimize or even avoid the need for bone grafting. These advanced solutions require a high level of surgical skill and are designed to utilize the patient’s existing bone structure in innovative ways.
Zygomatic Implants and Tilted Implant Concepts
For patients with extreme atrophy in the upper jaw (maxilla), zygomatic implants offer a graftless solution. These are much longer than traditional implants and are anchored into the dense zygomatic bone (cheekbone) instead of the jawbone. This provides an immediate, strong foundation for a full-arch restoration. Similarly, the All-on-4® or All-on-6® treatment concepts often utilize angled or tilted posterior implants. By tilting the implants, the surgeon can engage more of the available anterior bone, bypassing areas of deficiency and often avoiding the need for sinus lift procedures. To learn more about which option might be right for you, it is important to understand the best dental implant method for success based on individual anatomy and goals. These methods have revolutionized full-mouth rehabilitation, providing stable, fixed teeth for patients who were previously considered untreatable.