Dental Implants with Gum Disease
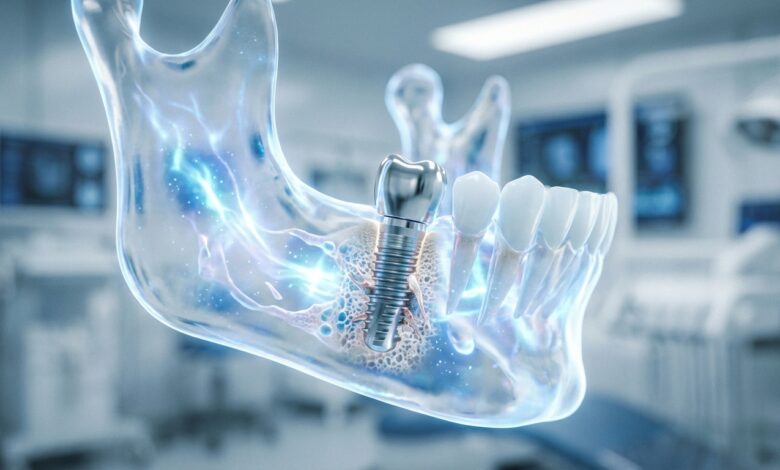
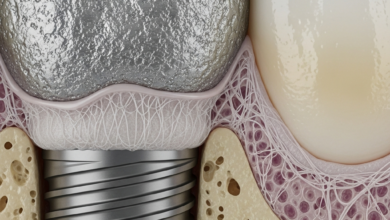
Before exploring the possibility of implants, it is essential to grasp what gum disease is and why it poses such a threat to any structure anchored in the jawbone. Gum disease is not a single condition but a spectrum of issues ranging from mild inflammation to severe tissue and bone destruction. The success of a dental implant is fundamentally dependent on a process called osseointegration, where the implant post fuses directly with the jawbone. Active gum disease directly undermines this foundational process.
What is Gingivitis and Periodontitis?
The journey of gum disease begins with gingivitis. This is the earliest and mildest form, caused by the buildup of plaque—a sticky film of bacteria—along the gumline. Symptoms include red, swollen gums that may bleed easily during brushing or flossing. The crucial thing to know about gingivitis is that it is entirely reversible with diligent oral hygiene and professional cleanings. The underlying bone and connective tissue are not yet affected.
If left untreated, gingivitis can progress to periodontitis. In this advanced stage, the inflammation spreads below the gumline. The body’s immune system responds to the bacterial toxins, and in this battle, the bone and connective tissues that hold teeth in place begin to break down. Gums pull away from the teeth, forming pockets that become infected. As periodontitis worsens, these pockets deepen, and more gum tissue and bone are destroyed. Eventually, teeth can become loose and may need to be removed. This same destructive process can attack a dental implant.
Why Active Gum Disease is a Contraindication for Implants
Placing a dental implant into a mouth with active periodontitis is setting it up for failure. The same bacteria that destroy the supporting structures of natural teeth will attack the support system of a dental implant. This condition, known as peri-implantitis, is the implant’s equivalent of periodontitis. The infection causes inflammation in the surrounding gums and leads to the progressive loss of the jawbone that anchors the implant. An implant without sufficient bone support will become loose and ultimately fail. Therefore, no reputable dental professional will proceed with implant surgery until any active gum disease is fully treated and under control.
The Critical Path: Treating Periodontitis Before Implant Surgery
The journey from having active gum disease to being ready for dental implants involves a systematic, multi-stage treatment process focused on eliminating infection and creating a stable oral environment. This phase is non-negotiable and is the most important factor in the long-term success of the implants.
Step 1: Professional Diagnosis and Assessment
The first step is a comprehensive periodontal examination. A dentist or a periodontist (a specialist in gum disease) will measure the depth of the periodontal pockets around each tooth using a probe. They will also take dental X-rays to evaluate the extent of bone loss. This assessment provides a clear picture of the severity of the disease and forms the basis of a tailored treatment plan. This evaluation determines if a patient is one of the ideal dental implant candidates or what steps are needed to get there.
Step 2: Non-Surgical Treatment (Scaling and Root Planing)
For most patients with mild to moderate periodontitis, treatment begins with a non-surgical procedure called scaling and root planing. This is often referred to as a “deep cleaning.” During scaling, the dentist removes all plaque and tartar (hardened plaque) from above and below the gumline, cleaning all the way down to the bottom of the pocket. Root planing involves smoothing the tooth roots to help the gums reattach to the teeth. This procedure is fundamental to removing the bacterial source of the infection and allowing the gums to heal.
Step 3: Surgical Interventions (If Necessary)
In cases of advanced periodontitis with deep pockets and significant bone loss, non-surgical treatment may not be enough. Surgical options might be required to fully restore gum health. These can include flap surgery (pocket reduction surgery), where the gums are lifted back to remove tartar, or bone and soft tissue grafts. Bone grafts are particularly relevant for future implant candidates, as they help regenerate some of the bone lost to the disease, creating a more solid foundation for the eventual implant.
Step 4: Re-evaluation and Maintenance Phase
After the initial treatment phase, a period of healing is necessary. The dentist will re-evaluate the health of the gums to ensure the infection has been resolved and the pockets have been reduced. This is not the end of the treatment. The patient then enters a maintenance phase, which is crucial for preventing the disease from recurring. This involves a strict at-home oral hygiene regimen and more frequent professional cleanings, typically every three to four months.
The Possibility of Dental Implants with Gum Disease History
Once the periodontal disease is successfully treated and stabilized, the conversation about dental implants can begin. A history of gum disease means a patient may have sustained permanent bone loss, which could affect the implant procedure. A thorough assessment, often involving a CT scan, will determine the quantity and quality of the existing jawbone. If there isn’t enough bone to support an implant, a bone grafting procedure may be necessary before the implant can be placed. The distinction between an active disease state and a controlled, historical condition is paramount.
| Feature | Active Gum Disease | Controlled Gum Disease (History) |
|---|---|---|
| Implant Candidacy | Not a candidate | Potentially a good candidate |
| Bone Health | Actively deteriorating due to infection | Stable, but may have reduced volume from past disease |
| Gum Tissue | Inflamed, bleeding, deep pockets present | Healthy, pink, firm, with no deep pockets |
| Bacterial Load | High levels of harmful periodontal bacteria | Normal, healthy oral flora |
| Immediate Next Step | Comprehensive periodontal treatment | Implant placement assessment and planning |
| Risk of Implant Failure | Extremely high due to peri-implantitis risk | Low, with diligent and consistent long-term maintenance |
Managing Long-Term Success: Preventing Peri-Implantitis
For a patient with a history of periodontitis, receiving dental implants is the beginning of a lifelong commitment to meticulous oral care. These individuals are inherently at a higher risk of developing peri-implantitis. The same factors that made them susceptible to gum disease can threaten their implants. Scientific studies have confirmed that a history of periodontitis is a significant risk factor for implant complications. A comprehensive review published on the National Center for Biotechnology Information website highlights the critical link between past periodontal disease and future implant health.
The Crucial Role of Patient Commitment
Long-term success rests heavily on the patient’s shoulders. The daily oral hygiene routine must be flawless. This includes brushing twice a day, focusing on the area where the implant meets the gumline. It also requires daily cleaning between the implant and adjacent teeth using specialized tools like implant-specific floss, interdental brushes, or a water flosser. These tools are essential for removing plaque from areas a normal toothbrush cannot reach.
The Importance of Professional Maintenance
Regular professional maintenance is just as important as at-home care. Patients with a history of gum disease should not follow the standard six-month check-up schedule. Instead, they typically require more frequent visits, often every three or four months. During these appointments, the hygienist will use special instruments made of plastic or resin to clean the implant surfaces without scratching them. The dentist will also regularly check the gum health around the implant, measure any pocket depths, and take periodic X-rays to monitor the underlying bone level, ensuring any early signs of trouble are caught and addressed immediately.