Signs of a Failed Dental Implant
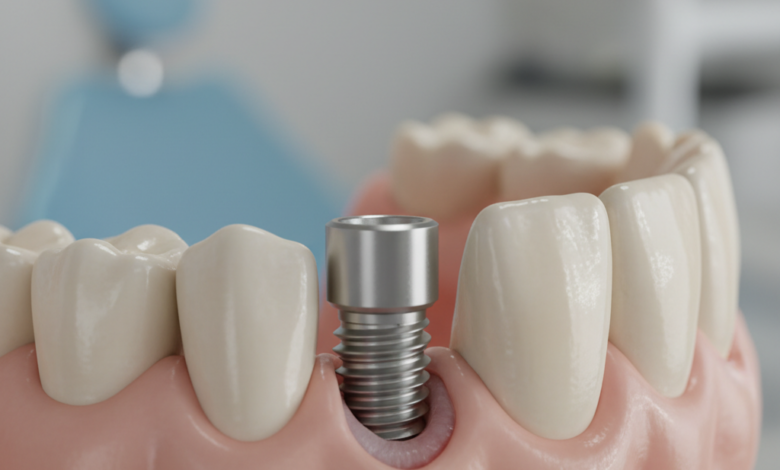
Signs of a Failed Dental Implant are often subtle at first but can escalate if not addressed promptly by a dental professional. While dental implants boast an exceptionally high success rate, often exceeding 95%, it is crucial for patients to understand that they are not immune to complications. A failed implant is a situation where the titanium post either fails to integrate with the jawbone—a process known as osseointegration—or loses its connection to the bone after a successful integration period. Recognizing the early warnings is the most effective way to mitigate damage, potentially save the implant site, and plan for a successful restoration. This detailed guide explores the causes, symptoms, and treatments associated with a failed dental implant, empowering you to protect your investment in your oral health.
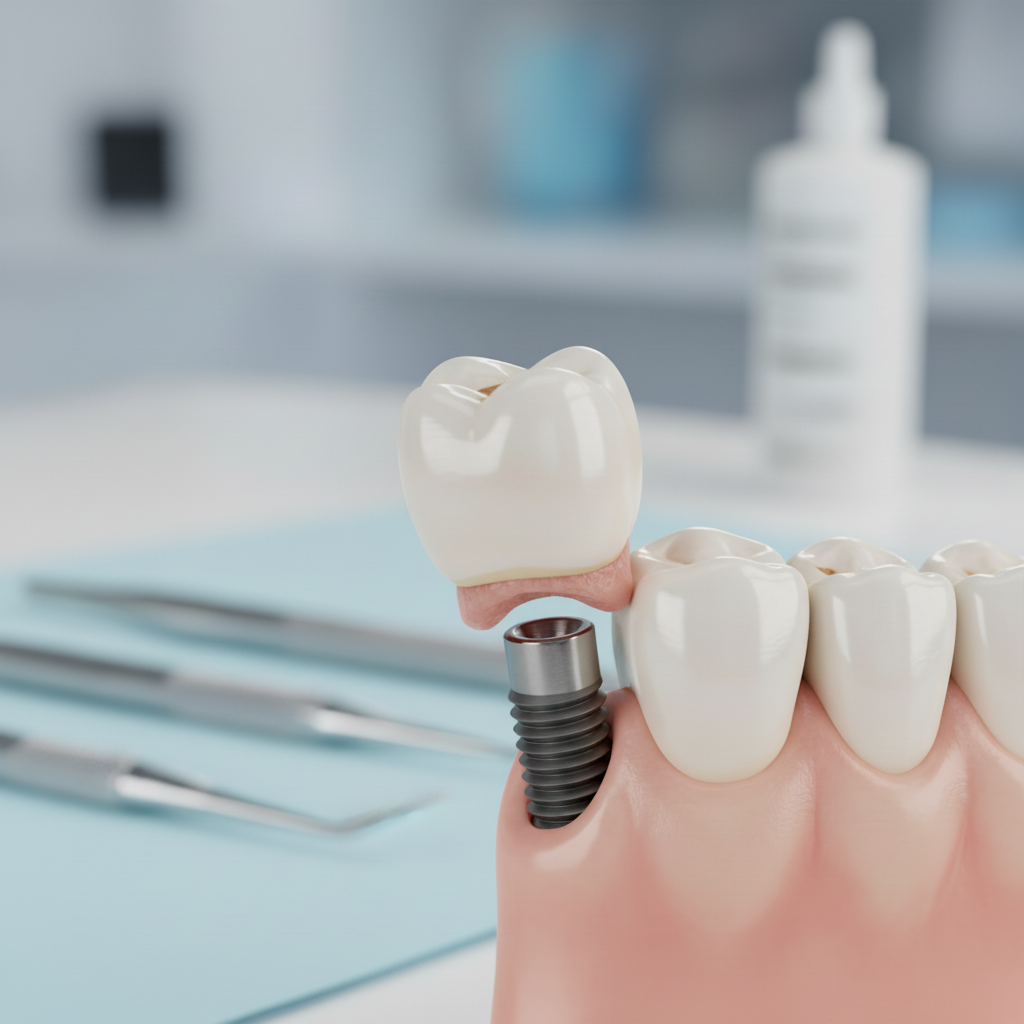
Understanding Dental Implant Failure: Early vs. Late Stage
Dental implant failure is not a single event but can be categorized into two primary timelines: early failure and late failure. Each has distinct causes and warning signs. Understanding this distinction is vital for both prevention and timely intervention.
Early implant failure occurs within the first few months after the implant placement surgery. The central issue during this period is the failure of the implant to properly fuse with the surrounding jawbone. This biological process, osseointegration, is the foundation of a stable and long-lasting dental implant. If this fusion is compromised for any reason, the implant will not be secure enough to support a crown and will ultimately fail.
Late implant failure can happen any time from one year to many years after the implant has been successfully integrated and restored with a crown. These failures are typically not related to the initial healing process but are caused by factors that develop over time. The most common culprit is a chronic infection or a sustained period of excessive mechanical stress on the implant fixture.
To provide a clearer understanding, the key differences are outlined below:
| Feature | Early Stage Implant Failure | Late Stage Implant Failure |
|---|---|---|
| Timing | Occurs within the first 3-4 months post-surgery. | Occurs anytime after one year post-surgery. |
| Primary Cause | Failure of osseointegration. Can be due to insufficient bone, infection, micro-movements of the implant, or patient health factors. | Often caused by peri-implantitis (a gum disease for implants), excessive biting forces, or mechanical failure of the implant components. |
| Key Symptoms | Significant pain, persistent swelling, mobility of the implant post during the healing phase. | Gum recession, pus or bleeding around the implant, deepening pockets, visible threads, or a loose crown. Pain may be absent in early stages. |
| Treatment Approach | The implant is typically removed. The site is cleaned, and a bone graft may be necessary before a new implant can be attempted after a healing period. | Treatment depends on severity. It may involve deep cleaning, gum surgery, or, in advanced cases, implant removal and site reconstruction. |
The Most Common Reasons for a Failed Dental Implant
The success of a dental implant hinges on a delicate balance of biological, mechanical, and patient-specific factors. When this balance is disrupted, failure can occur. Delving into the specific causes can help patients and clinicians create a more robust strategy for long-term success.
Peri-Implantitis: The Silent Threat
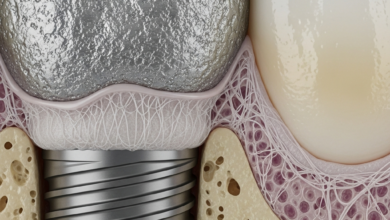
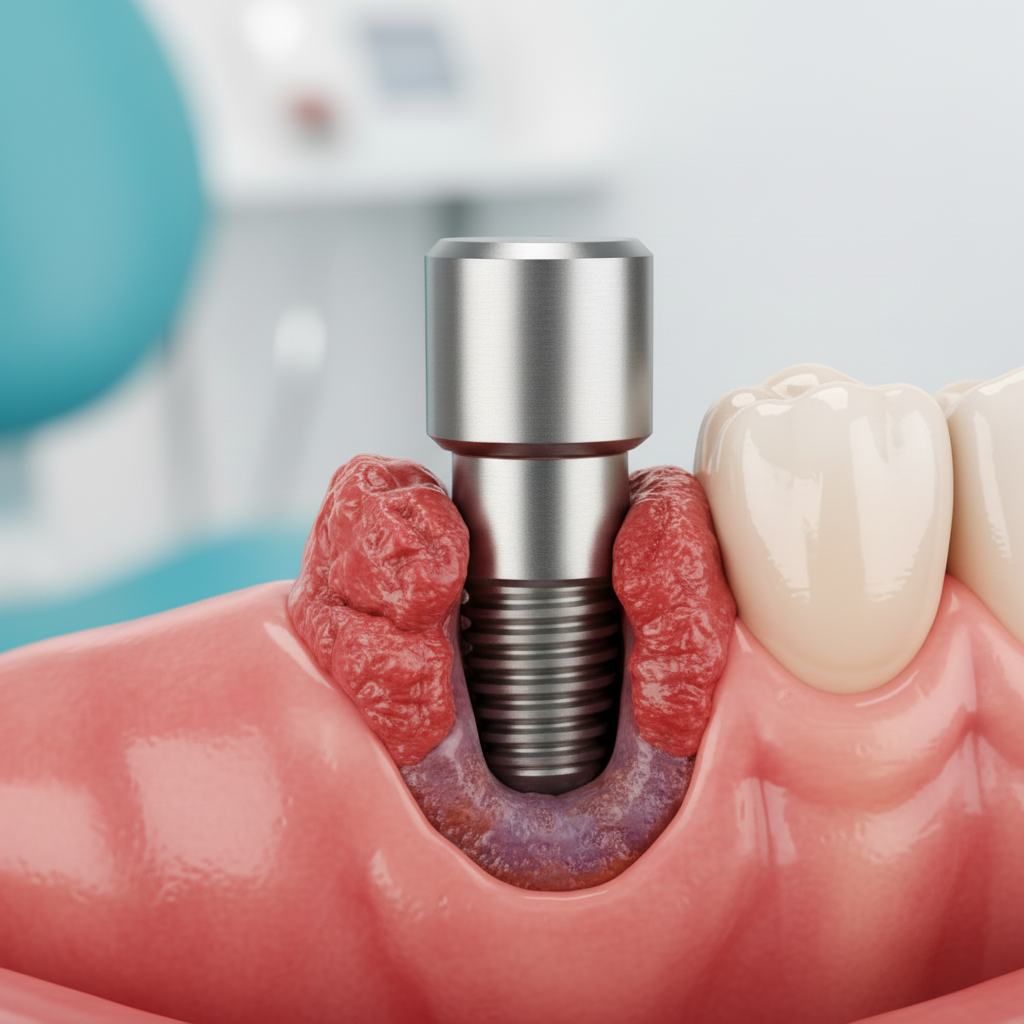
By far the most common cause of late-stage implant failure, peri-implantitis is an inflammatory condition affecting the gum and bone tissue surrounding a dental implant. It is essentially the implant equivalent of periodontal (gum) disease. The process begins with mucositis, which is inflammation of the soft tissues, often characterized by red, swollen gums that may bleed upon brushing. If left untreated, mucositis can progress to peri-implantitis, where the inflammation leads to the gradual destruction of the bone supporting the implant. This bone loss compromises the implant’s stability, causing it to become loose and eventually fail. Poor oral hygiene is the primary driver, as it allows harmful bacteria to accumulate around the implant base.
Failed Osseointegration
This is the cornerstone of early implant failure. Osseointegration is the remarkable process where bone cells grow directly onto the biocompatible titanium surface of the implant, locking it firmly into the jaw. Several factors can hinder this critical process:
- Insufficient Bone Density or Volume: An implant needs a certain amount of healthy bone to anchor it securely. If the bone is too thin or soft, it cannot provide the necessary stability for integration. This is why a bone grafting procedure is often recommended before implant placement in patients with significant bone loss.
- Premature Loading: Placing excessive pressure on the implant, such as attaching a permanent crown too early, can cause micro-movements that disrupt the delicate process of bone cells attaching to the implant surface.
- Systemic Health Issues: Certain medical conditions, like uncontrolled diabetes or autoimmune diseases, can impair the body’s natural healing abilities, making successful osseointegration more challenging.
Poor Surgical Technique or Planning
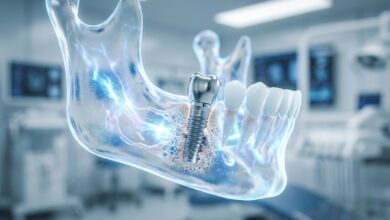
The experience and skill of the surgeon are paramount. An improperly positioned implant can be subjected to unnatural forces, leading to mechanical stress and bone loss over time. Likewise, overheating the bone during the drilling process can damage the surrounding bone cells, preventing them from integrating with the implant. Careful pre-surgical planning using 3D imaging (CBCT scans) is essential to map out nerves, sinuses, and available bone, ensuring a precise and safe placement. A comprehensive overview of potential issues is vital; as detailed in an article about dental implant complications explained, proper planning minimizes these risks.
Identifying the Symptoms of Implant Failure
Vigilance is key to early detection. While some symptoms are obvious, others can be subtle. If you experience any of the following, it is imperative to contact your dentist immediately.
Persistent Pain and Discomfort
While some discomfort is normal immediately following surgery, it should gradually subside. Severe, throbbing, or persistent pain that continues weeks or months after the procedure is a major red flag. This could indicate an underlying infection or a failure of the implant to integrate with the bone.
Implant Mobility
A successfully integrated dental implant should be as solid and stable as a healthy natural tooth. There should be zero movement. If you can feel the implant post or the crown wiggling or shifting, it is a definitive sign of failure. This mobility indicates that osseointegration has not occurred or has been lost.
Swelling and Inflammation of the Gums
Gums that are persistently red, puffy, or swollen around the implant area are a classic sign of inflammation. This is often the first symptom of peri-mucositis or the more severe peri-implantitis. You might also notice bleeding when you brush or floss around the implant.
Difficulty Chewing or Biting
Pain or a feeling of unease when you bite down can indicate a problem. This could be due to a loose crown or, more seriously, a mobile implant that is shifting under pressure. It can also suggest that the implant is not positioned correctly and is absorbing too much bite force.
What to Do and How to Prevent Failure
If you suspect your implant is failing, the first and only step is to schedule an immediate appointment with your dental surgeon. Do not wait for the symptoms to worsen. During the visit, the dentist will perform a thorough clinical examination, check for mobility, measure the gum pockets around the implant, and take X-rays to assess the bone level.
The treatment for a failed implant depends entirely on the cause and severity. If the issue is a loose abutment or crown, it can often be tightened or replaced. However, if the implant post itself has failed to integrate or has lost significant bone support due to peri-implantitis, it will likely need to be removed. After removal, the site must be meticulously cleaned of all infected tissue. A bone graft is often necessary to rebuild the lost bone structure. Once the site has fully healed, which can take several months, a new implant may be placed.
Prevention remains the best strategy. The risk of implant failure is significantly influenced by patient-related factors. According to a study published in the National Center for Biotechnology Information, factors like smoking and a history of periodontitis are significant risk indicators. To ensure the longevity of your implant, adhere to the following:
- Impeccable Oral Hygiene: Brush twice a day and floss daily. Special tools like water flossers or interdental brushes are highly effective for cleaning around an implant.
- Regular Dental Check-ups: Professional cleanings and examinations every six months allow your dentist to monitor the implant and catch any early signs of trouble.
- Avoid Smoking: Smoking restricts blood flow, which impairs healing and increases the risk of infection and implant failure.
- Manage Systemic Health: Keep conditions like diabetes under control to support your body’s ability to maintain healthy bone and gum tissue.
A dental implant is a significant investment in your health and quality of life. By understanding the potential signs of failure and committing to diligent care, you can protect that investment and enjoy a stable, confident smile for decades to come.